9.8 Antiemetics V2
Nausea is a common condition that can occur temporarily and be self-limiting to more chronic conditions which can be very debilitating. For a review of causative factors of nausea, refer to unit 9.3 Conditions and Diseases of the Gastrointestinal System. For severe cases of vomiting, intravenous fluids may also be needed to treat the accompanying dehydration (Medline Plus, 2019; Bashashati, & McCallum, 2014). The treatment of nausea and vomiting should be tailored to the causative factor. There are several medications that work on different neuroreceptors that can treat nausea and vomiting. Table 9.8 compares the neurotransmitters involved in the nausea and vomiting process, classes of antiemetic medication targeting these neurotransmitters, prototype antiemetic medications, and associated mechanisms of action (Bashashati, & McCallum, 2014; Garrett et al, 2003; Sealock & Seneviratne, 2021). Each medication class is also discussed in more detail later in this section.
| Neurotransmitter | Medication Class | Antiemetic Drug | Mechanism of Action |
| Acetylcholine (M1) | Anticholinergics | Scopolamine | Blocks ACh receptors in vestibular system |
| Histamine (H1) | Antihistamines | Meclizine, Dimenhydrinate, Diphenhydramine | Blocks H1 receptors and thus blocks ACh in vestibular system |
| Dopamine (DA2) | Dopamine 2 antagonists | Prochlorperazine, Promethazine | Blocks dopamine in CTZ and also block ACh |
| Dopamine and ACh (DA2 and M1) | DA2 + Prokinetics | Metoclopramide | Blocks dopamine in CTZ and stimulates ACh in GI tract |
| Serotonin (5HT) | Serotonin antagonists | Ondansetron | Blocks serotonin in GI tract, CTZ, and VC |
| Substance P (NK1) | Neurokinin antagonists | aprepitant | Inhibits substance P neurokinin receptors |
| Cannabinoid (CB1) | Tetrahydrocannabinols (THC) | dronabinol or medical marijuana | Activated CB1 receptor leading to inhibitory effects on cerebral cortex, reticular formation & thalamus. |
Antiemetic Medication Classes
Anticholinergics
Scopolamine is an example of an anticholinergic medication that is often used to treat motion sickness or nausea and vomiting associated with recovery from anesthesia and/or opiate analgesia.
Mechanism of Action
Anticholinergics block acetylcholine (ACh) receptors in the vestibular center and within the brain to prevent nausea-inducing stimuli to the Chemoreceptor Trigger Zone (CTZ) and the Vomiting Center (VC). They also block receptors in the reticular formation, preventing Ach binding to these receptors and therefore stop the signals to the VC. Due to the anticholinergic effects, they also dry GI secretions and reduce smooth muscle spasms.
Administration Considerations
The scopolamine transdermal patch (see Figure 9.7a) is designed for continuous release of scopolamine following the application to an area of intact skin on the head, behind the ear. The system is formulated to deliver approximately 1 mg of scopolamine to the systemic circulation over 3 days.
Possible side effects and contraindications:
- Due to its anticholinergic properties, scopolamine can decrease gastrointestinal motility and cause urinary retention. Monitor client and discontinue with client reports difficulty urinating.
- Other side effects: constipation, blurred vision, flushing
- Adverse effects: exacerbate psychosis, induce seizures, and cause drowsiness, confusion, and sedation.
- contraindicated in clients with glaucoma.
- Clients going for MRI: Transderm Scōp contains an aluminized membrane; skin burns have been reported at the application site in clients wearing an aluminized transdermal system during an MRI scan. Remove patch before undergoing an MRI.
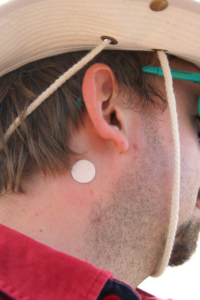
Andrea’s note: From current OER
Application instructions:
- Only wear one transdermal system at any time.
- Do not cut the transdermal system.
- Apply the transdermal system to the skin in the postauricular area (hairless area behind one ear).
- After the transdermal system is applied on the dry skin behind the ear, wash hands thoroughly with soap and water and dry hands.
- If the transdermal system becomes displaced, discard the transdermal system, and apply a new transdermal system on the hairless area behind the other ear.
- For surgeries other than caesarean section, apply one Transderm Scōp transdermal system the evening before a scheduled surgery. Remove the transdermal system 24 hours following surgery (Riad & Hithe, 2023).
Client Teaching
- Ensure clients are aware of potential side effects or adverse effects.
- May impair the mental and/or physical abilities required for the performance of hazardous tasks such as driving a motor vehicle, operating machinery, or participating in underwater sports.
- Concomitant use of other drugs (e.g., alcohol, sedatives, hypnotics, opiates, and anxiolytics) that cause central nervous system (CNS) adverse reactions, or that have anticholinergic properties, may increase this impairment. Inform clients not to operate motor vehicles or other dangerous machinery or participate in underwater sports until they are reasonably certain that Transderm Scōp does not affect them adversely.
- Can cause temporary dilation of the pupils resulting in blurred vision if it comes in contact with the eyes. Advise clients to wash their hands thoroughly with soap and water and dry their hands immediately after handling the patch.
- Upon removal, fold the used transdermal system in half with the sticky side together, and discard in household trash in a manner that prevents accidental contact or ingestion by children, pets, or others (Riad & Hithe, 2023).
Antihistamines
Meclizine is an example of an antihistamine that is often used to treat motion sickness. Other antihistamines include Dimenhydrinate and Diphenhydramine. Diphenhydramine (trade name: Benadryl) is used for many purposes besides nausea such as allergy symptoms and rhinitis. Dimenhydrinate (trade name: Gravol) is used extensively for treating nausea and vomiting. Many antihistamines are available orally OTC.
Mechanism of Action
Antihistamines inhibit the action of histamine at the H1 receptors in the vestibular center. They also block H1 receptors located in nerves, smooth muscle and glands. Further, antihistamines have potent anti-cholinergic activity blocking acetylcholine at the muscarinic receptors in the reticular formation and vestibular nuclei, which leads to many of the side effects experienced by clients.
Nursing Considerations
Antihistamines are a relatively safe medication, used extensively both as an OTC option and in hospital settings.
Given oral, IV, IM. Well absorbed orally.
Motion sickness: dosage should be started one hour before travel begins.
Crosses the placenta, avoid in pregnancy.
Caution with the older adult; may develop agitation, confusion and hypotension.
Potential Side effects:
- Dry mouth, slower gastric motility (constipation), urinary retention, sedation, drowsiness.
- Some health conditions are contraindicated with antihistamines:
- clients with narrow angle glaucoma as it can lead to blurred vision
- benign prostate hypertrophy (enlarged prostate gland) as it can lead to further urinary retention
- COPD as antihistamines will dry bronchial passages leading to decreased ability to cough up secretions (Sealock & Seneviratne, 2021).
Client Teaching
- Do not exceed recommended dosage.
- Be advised that drowsiness may occur. Due to drowsiness, refrain from driving a motor vehicle or operating machinery.
- Avoid alcohol, sedatives, and tranquilizers, which may increase drowsiness.
Dopamine Antagonists
Phenothiazine is a broad antidopaminergic drug classification with two drugs: promethazine and prochlorperazine. Both are used to treat nausea and vomiting and used commonly in acute care settings. They are used for nausea related to surgery, chemotherapy, migraines, vertigo and even hiccups. Chlorpromazine, under the same antidopaminergic category, has been used as an antipsychotic medication to treat bipolar and schizophrenia. Off label, promethazine can also be used for its sedating properties as it blocks H1 receptors in the brain.
Our prototype medication will be promethazine
Mechanism of Action
Phenothiazine blocks dopamine in the Chemoreceptor Trigger Zone (CTZ). It also has antihistaminergic and anticholinergic effects.
Administration Considerations
Administration: oral, IM or IV.
- It is preferred to be given oral or IM. Deep IM injection as SQ will damage tissue.
- Give with food, water or milk to decrease GI discomfort.
- IV route: extreme caution as if it goes interstitial, tissue necrosis can occur. Only use a large bore IV with a running IV line. Tell client to report any burning at the site, and stop the infusion immediately.
Used for short term therapy due to risk of tardive dyskinesia with long term use.
Contraindicated in clients with:
- Movement disorders such as seizures, Parkinson’s disease.
- encephalopathy, comatose, dementia
- bone marrow depression.
Contraindicated with:
- the older adult due to neuro side effects.
- in children under age 2 or under 20 pounds. Due to sedating properties, can cause respiratory depression.
May be given in pregnancy for difficult-to-treat nausea.
Side effects: sedation, confusion, disorientation. Anti-cholinergic effects such as dry mouth, urinary retention and constipation.
Adverse effect: neuroleptic malignant syndrome – rare but potentially fatal adverse effect (cues: hyperpyrexia, altered mental status, muscle rigidity, and autonomic instability)
Client Teaching
- Instruct to take medications as prescribed.
- Avoid alcohol and other CNS depressants.
- May experience increased photosensitivity
Sealock & Seneviratne, 2021; Southhard & Al Khalili, 2024
Dopamine 2 Antagonist and Prokinetics
Jessica / Nov 17, 2025: Hyperlinks below point to version 1 of the book.
Prokinetics are named as they get the GI tract moving. It enhances GI motility by promoting peristalsis and enhances GI emptying. Metoclopramide is an example of a prokinetic medication (see Figure 9.8b). It has both dopaminergic antagonist and prokinetic action. By promoting peristalsis, it can help alleviate nausea and treats a wide range of nausea-related conditions. It is beneficial for clients with delayed gastric emptying and in treating GERD symptoms. It is also used to treat nausea in post op and chemotherapy clients. It can be used off-label for pregnant women with hyperemesis gravidarum. For severe migraines, it has also been shown to be effective.
It is a prescription only medication due to the risk of adverse effects.
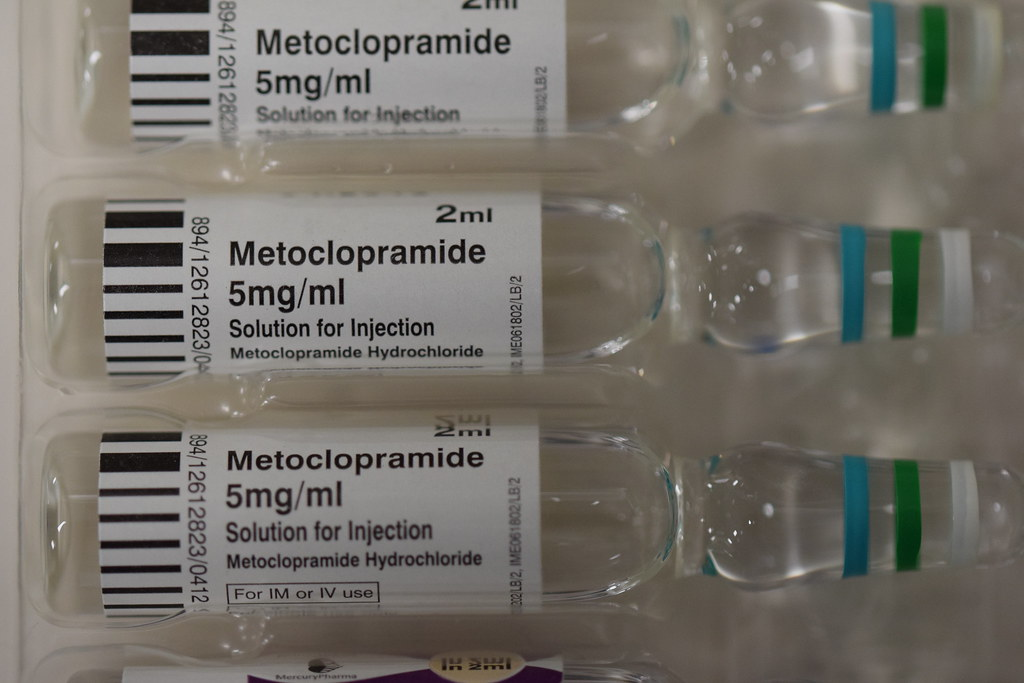
Andrea’s note: image from current OER
Mechanism of Action
The primary action of metoclopramide is that it blocks central and peripheral dopamine 2 receptors in the CTZ, which desensitizes the CTZ to impulses it receives from the GI tract. As an prokinetic, it has a number of actions. It is an antagonist to 5HT3 (type 3 serotonin receptors) and an agonist at 5HT4 receptors. It also blocks the anti-peristaltic effects of apomorphine, leading to an acceleration of gastric emptying. It also increases the tone of the esophageal sphincter and relaxes the pyloric sphincter, leading to increased peristalsis action (Isola et al, 2023).
Administration Considerations
Administer Oral, IM or IV. Metoclopramide is lipid-soluble, giving it a large half-life and a large volume of distribution. Its half-life can range from 4.5 hours to 8.8 hours. It is typically used short term use only.
- IV onset of action is 1-3 minutes
- IM onset of action 10-15 minutes
- Oral onset of action 30-60 minutes
It has a long t1/2 ranging from 4.5 to 9 hours, thus a long duration of action. Any renal impairment will prolong its effects.
Do not use if stimulation of GI motility might be dangerous (e.g., in the presence of gastrointestinal hemorrhage, mechanical obstruction, or perforation).
Side effects include:
- Orthostatic Hypotension
- Sedation
- Headache
- Dry mouth, diarrhea
Adverse effects:
- Risk of extrapyramidal effects including tardive dyskinesia with long term use.
- Do not take if already taking meds that have potential to cause extrapyramidal effects such as antipsychotics and tricyclic antidepressants.
- Rare: neuro-malignant syndrome
Contraindicated in clients with:
- pheochromocytoma – may cause hypertensive crisis.
- epilepsy or clients with movement disorders (ie. Parkinson’s disease)
- older adult especially due to orthostatic hypotension
Client Teaching
- Advise client of side effects and adverse effects
- Avoid with other meds that may cause sedation such as alcohol or sedatives.
- Teach clients to immediately inform the healthcare provider if they experience new feelings of depression or abnormal muscle movements they cannot control such as:
- lip-smacking, chewing, or puckering of the mouth
- frowning or scowling
- sticking out the tongue
- blinking and moving the eyes
- shaking of the arms and legs
Go to the website: What is Tardive Dyskinesia: https://www.tardiveimpact.com/what-is-td
Andrea’s note: Jessica – Not sure if I can use this website, in particular the videos that show TD
Jessica/ Nov 17, 2025: @Copyreditor could you please advise if link, particularly the video, can be use above?
Serotonin Receptor Antagonists
Ondansetron is an example of a serotonin (5HT) antagonist often used to treat severe nausea and vomiting associated with chemotherapy, postoperative nausea and vomiting, and hyperemesis during pregnancy. It is not effective against motion sickness. Ondansetron is considered a safe, well tolerated medication with minimal side effects. It is available by prescription only and is more costly than other options. As such, for clients at home, it is typically prescribed when other anti-emetics have been tried and not successful.
See Figures 9.8c and 9.8d for images of the injectable and oral formulations of ondansetron.
Andrea’s note: Both images from current OER
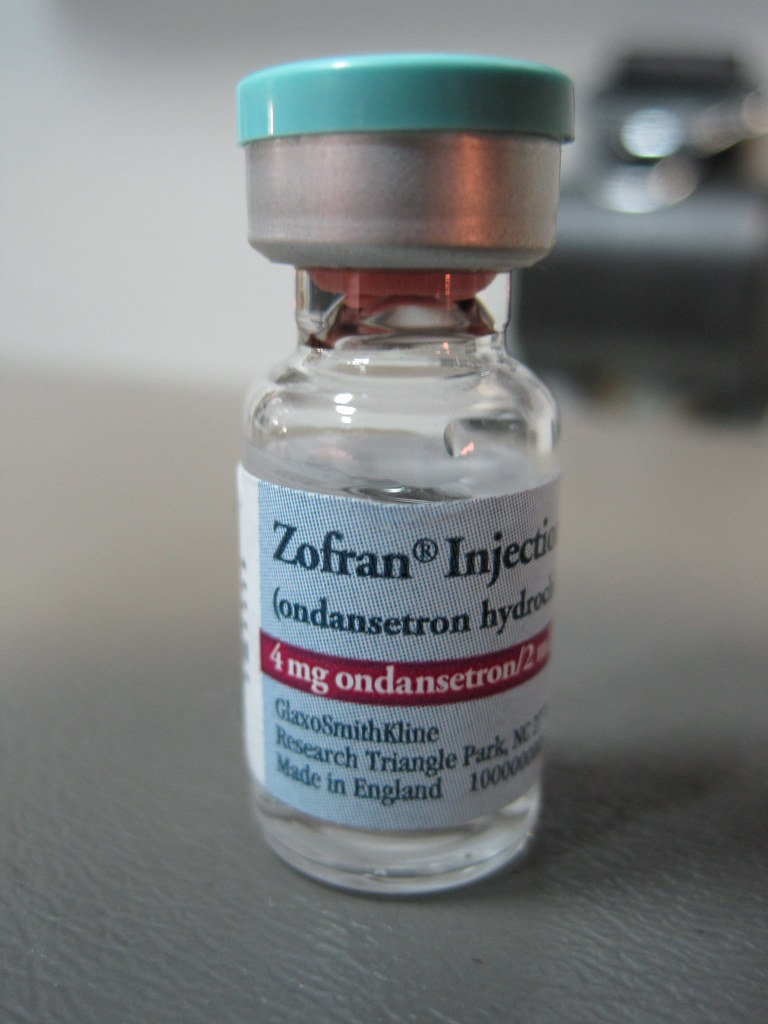
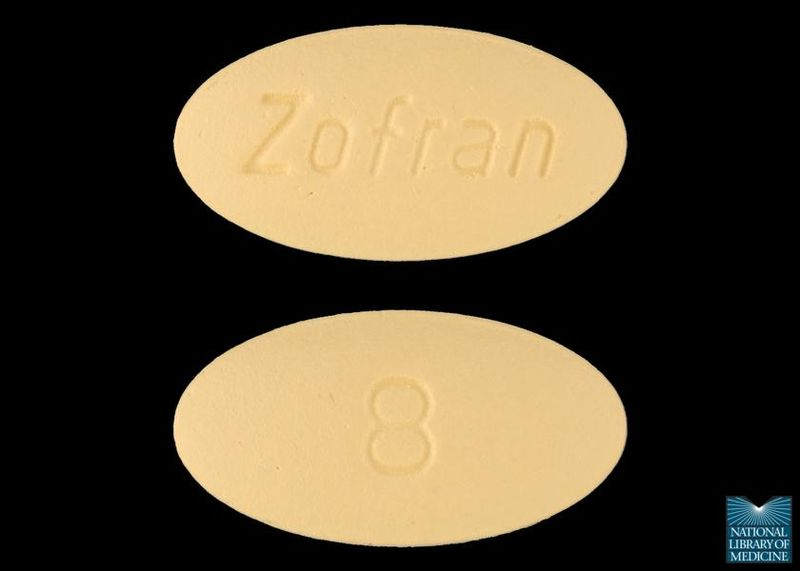
Mechanism of Action
Ondansetron blocks serotonin receptors in the small bowel, vagus nerve and the chemoreceptor trigger zone (CTZ). This action then decreases the afferent visceral and CTZ stimulation of the vomiting center (VC). Because of the diffuse blocking of serotonin, ondansetron is effective for many causes of nausea.
(See Figure 9.8e for an image of ondansetron blocking the 5-HT3 receptor.[13])
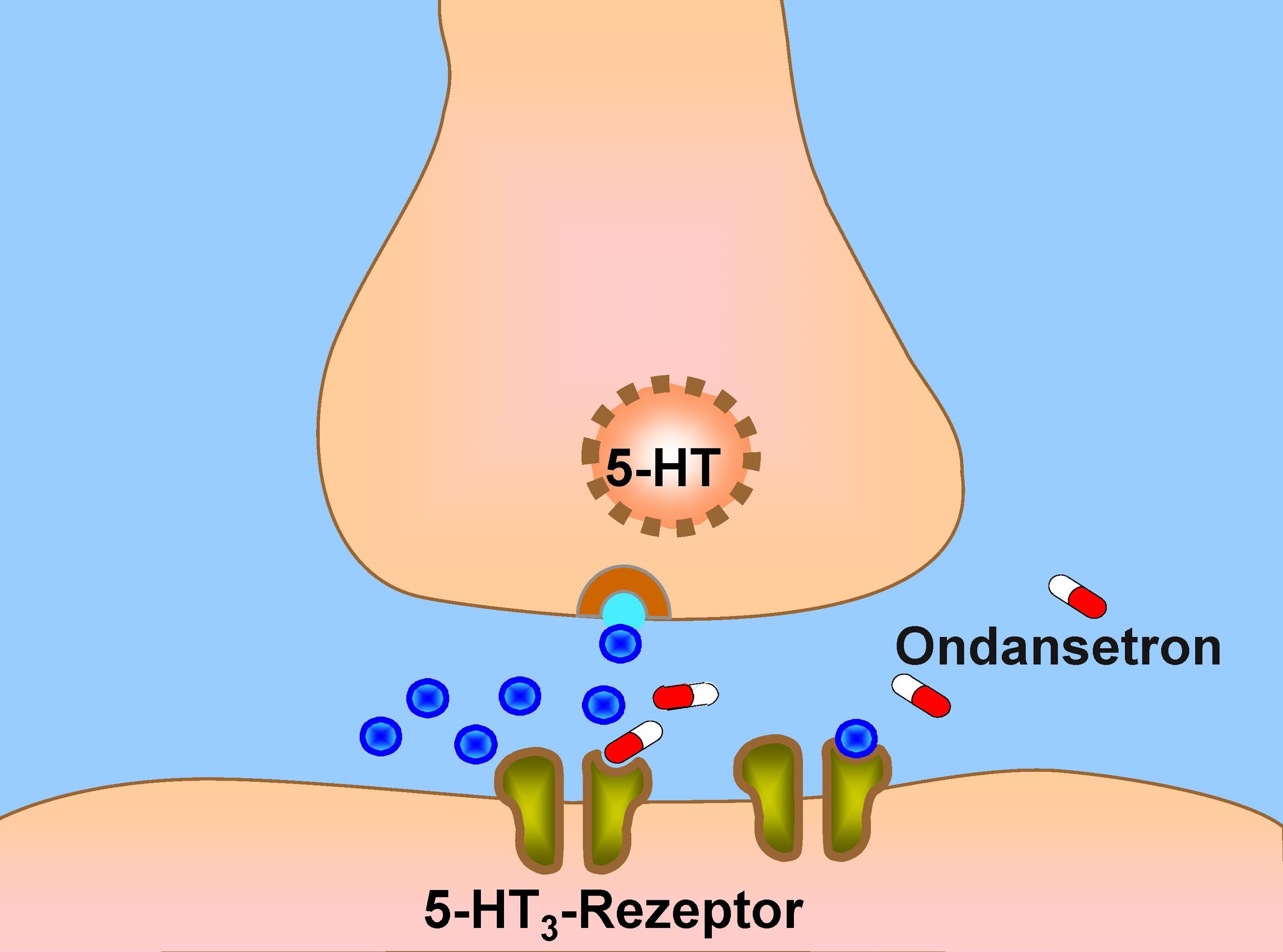
Andrea’s note: from current OER
Administration Considerations
Ondansetron is available as an orally disintegrating tablet, intramuscularly, and as an injectable for those clients too nauseated to tolerate oral medication. It is well tolerated and very effective. Side effects include:
- Headache is a primary side effect
- Fatigue, drowsiness
- Constipation, diarrhea
- Fever
Other adverse effects, albeit rare, can include hypersensitivity reactions and transient elevation of liver enzymes. Also rare, is the asymptomatic QT prolongation and QRS widening (Flake, Scalley & Bailey, 2004). Older adults and clients with any cardiac issues, electrolyte imbalances or taking other meds that also prolong QT interval, may be more susceptible to the ECG changes and subsequent risk of torsade’s de pointes. When giving ondansetron regularly and in higher doses, closer monitoring may be required (Singh et al, 2023).
Clients that take other serotonin antagonists or selective serotonin reuptake inhibitors (antidepressant), can have a risk of Serotonin syndrome.
It can be used for pediatric and adult clients. For children, it is prescribed for gastroenteritis, and particularly effective is the dissolvable tablet. It can also be prescribed for first trimester pregnancy although there is inconclusive evidence of its safety for the fetus (Flake, Scalley & Bailey, 2004).
Client Teaching
Ondansetron has side effects that affect the CNS, cardiovascular and gastrointestinal systems. Clients should be well-informed of these potential effects and take necessary precautions. Teach clients to immediately inform their healthcare provider if they experience:
- heart rate change, light-headedness,
- dizziness,
- hypersensitivity reactions such as fever, chills, rash, or breathing problems
Other side effects such as diarrhea or constipation and headache are usually mild and self-limiting.
(Griddine & Bush, 2023).
Neurokinin Receptor Antagonists
Aprepitant is an example of a neurokinin antagonist used to prevent nausea and vomiting associated with chemotherapy and surgery. It also has anxiolytic and antidepressant properties. It is used as part of an anti-emetic regime, especially for clients undergoing chemotherapy. It is taken orally or by intravenous. Due to being so costly, it is only used in hospital or clinic settings.
Mechanism of Action
Aprepitant, a NK-1 receptor antagonist, competitively binds to the NK-1 receptor, thereby blocking the binding of substance P and preventing the transmission of the emetic signal. It is highly selective in crossing the blood-brain barrier to occupy NK-1 receptors in the brain.
Administration Considerations
Aprepitant is usually administered concurrently with dexamethasone (a corticosteroid) and ondansetron. It can be administered orally or intravenously.
Onset of action: one hour, with a peak effect in four hours, so it is not used for immediate anti-emetic relief, but for anticipatory nausea.
Anticipatory nausea: The duration of action of up to 40 hours makes this med ideal for managing the persistent nausea experienced with chemotherapy.
It is not approved for pregnancy or pediatric populations.
Aprepitant is renally excreted, so dose adjustments are required (Ibrahim, Pellegrini, & Preuss, 2023).
Drug Interactions
It has clinically significant CYP3A4 drug interactions with medications such as pimozide, diltiazem, and rifampin, and can decrease INR levels when taken concurrently with warfarin. It can also reduce the effectiveness of oral contraceptives. (Ibrahim, Pellegrini, & Preuss, 2023).
Aprepitant is metabolized by P450 in particular by CYP3A4, as well as CYP1A2 and CYP2C19. Numerous drug interactions can occur, so prescribers will do a comprehensive review of all medications to minimize or eliminate any drug interactions. Nurses need to complete a thorough medication profile with the client including OTC or herbal remedies (Ibrahim, Pellegrini, & Preuss, 2023).
Side Effects
Aprepitant side effects are mild and can include sleepiness, diarrhea, weakness, constipation, stomach pain, heartburn, nausea, hiccups, loss of appetite, headache, fever, itching, and hair loss.
Rarely, more severe adverse reactions can occur and include hypersensitivity reactions such as a rash, Stevens-Johnson syndrome or angioedema.
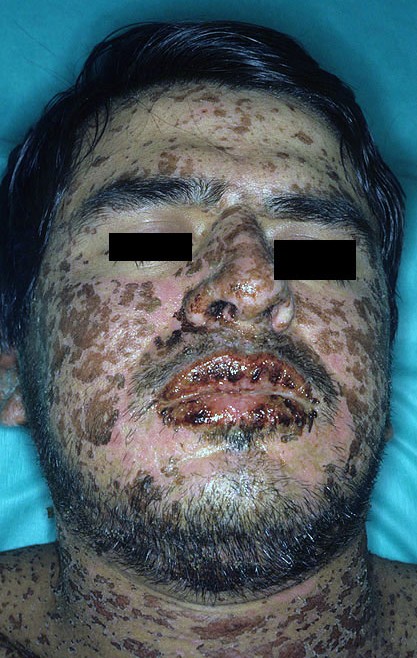
Figure 9.8f Steven-Johnson Syndrome rash
Photo Link: https://commons.wikimedia.org/wiki/File:Stevens-johnson-syndrome.jpg
Client Teaching
Advise client to take aprepitant as directed.
Ensure the client is aware of any potential side effects and to report immediately any hypersensitivity reaction such as a rash, angioedema, itching or difficulty breathing.
Many drug interactions can occur. Ensure the client reports any new medications, including OTC, herbal remedies or vitamins. Some drug interactions that require specific teaching include:
- Warfarin – NK-1 antagonists taken along with warfarin can lead to a decreased warfarin effect, and subsequently a higher risk of clot formation. Advise clients to monitor their INR levels more closely, which may require adjustment of the warfarin dosage while taking aprepitant.
- Oral contraceptives – NK-1 receptor antagonists may diminish the effectiveness of oral contraceptives. Advise the client to use a back-up pregnancy protection method, and continue with these measures for one month after discontinuing therapy (Ibrahim, Pellegrini, & Preuss, 2023).
Tetrahydrocannabinoids (THC)
Jessica / Nov 17, 2025: Hyperlinks below point to version 1 of the book.
Dronabinol and nabilone are synthetic THC along with medical marijuana are examples of a THC medications used to treat nausea, in particular clients with cancer or palliation when more conventional treatments have not been successful (see Figures 9.7f and 9.7g). It is also used for many other health issues including chronic pain relief, reducing spasticity related to spinal cord injury, seizure disorders, mental health conditions (depression and anxiety), and stimulating appetite (Sealock & Seneviratne, 2021).
Nabilone, another derivative of THC, is more potent than dronabinol and is used as well for the treatment of chemotherapy induced nausea. Both medications are relatively safe, but dizziness, hypotension, euphoria, ataxia and dry mouth are commonly reported side effects (Drugs.com, 2025).

Andrea’s note: images from current OER
Mechanism of Action
There is a great deal we are still learning about the effects of cannabinoids and its mechanism of action. Its anti-emetic effects are related to the inhibitory effects on the reticular formation, thalamus and cerebral cortex and through activating cannabinoid receptors in and around the vomiting center. Other effects might include antagonistic effects at 5-HT3 receptors in the brain (Sealock & Seneviratne, 2021).
Administration Considerations
As a lipophilic drug, Nabilone and Dronabinol cross the blood brain barrier and can cause dizziness, vertigo, and the dose-related “high” (easy laughing, elation, and heightened awareness). Although both of these products can produce some of the intoxicating effects similar to cannabis, they have a low abuse potential due to the slow onset of action. There is a risk of being abusable, and as such are a prescription medication.
Older adult: THC should be used cautiously in older adult clients because they may be more sensitive to the neurological, psychoactive, and postural hypotensive effects of the drug. In general, dose selection should be cautious, usually starting at the low end of the dosing range.
Pregnancy and Breastfeeding: THC should not be used while pregnant. Neonates are at risk for fetal growth restriction, low birth weight, and small for gestational age. THC passes through breastmilk, and although studies are limited, it is advised to sustain from breastfeeding for nine days after using THC (Drugs.com, 2025).
Client Teaching
THC has side effects that affect the CNS, GI, and cardiovascular systems. Clients should be well-informed of these potential effects and take necessary precautions.
- Avoid drinking alcohol as it can potentiate dizziness and drowsiness effects.
- Clients should not drive, operate machinery, or engage in any hazardous activity when using THC.
- Keep out of reach of children and pets.
- Nabilone can lead to psychological or physical dependence; use only as needed to treat nausea.
- Drug interactions are common, discuss with prescriber before starting medical cannabis or one of the prescribed medications.
Herbal and Vitamin Supplements
Herbal remedies have been used historically and still used today to treat nausea as part of traditional healing practices. For example, ginger has been used in traditional Indian and Chinese medicine as an antiemetic. Interestingly, 80% of the world population rely on traditional remedies or medicinal plants to treat not only nausea but many ailments. Although we are only highlighting a few herbal remedies, there are many others including cinnamon, lavender, and citrus (Mohsenzadeh et al, 2018).
There is a public perception that herbal remedies are safe, but there can be adverse effects, especially if used along side pharmaceutical medications. A nurse’s responsibility is to inform the client of potential risks if taking other medications and to recognize that all medications, including herbal supplements can cause side effects.
Herbal remedies have been used historically and still used today to treat nausea as part of traditional healing practices. For example, ginger has been used in traditional Indian and Chinese medicine as an antiemetic. Interestingly, 80% of the world population rely on traditional remedies or medicinal plants to treat not only nausea but many ailments. Although we are only highlighting a few herbal remedies, there are many others including cinnamon, lavender, and citrus (Mohsenzadeh et al, 2018).
There is a public perception that herbal remedies are safe, but there can be adverse effects, especially if used along side pharmaceutical medications. A nurse’s responsibility is to inform the client of potential risks if taking other medications and to recognize that all medications, including herbal supplements can cause side effects.
Ginger
Ginger is a well-known antiemetic. Although its mechanism of action is not completely understood, ginger is thought to antagonize the 5HT and cholinergic receptors and may have direct effect on the gastrointestinal tract. Although ginger can cause reflux and heartburn and may potentially cause bleeding because of its anticoagulant effects, dosages of up to 2 g per day in divided doses of 250 mg are considered safe, even in pregnant women.
Ginger can be taken in different forms. Tablets or capsules are convenient and are easily available at most pharmacies and health food stores. Other options are ginger tea or ginger candies if swallowing a capsule is not ideal.

Pyridoxine (vitamin B6)
Pyridoxine has also been recommended for treating nausea and vomiting in pregnancy. Typical dosages of pyridoxine, 10 to 25 mg every eight hours, cause minimal adverse effects (Mohr et al, 2021).
Peppermint
Peppermint can help relax the muscles in the digestive tract and can ease the nausea symptoms. It can be used as aromatherapy and has shown some benefit to reducing nausea. It can also be consumed in a tea or in a lozenge. Side effects of peppermint are typically minor and include acid reflux (Mohr et al, 2021).

Comparing Antiemetics Medication Table
Now let’s take a closer look at the Chapter 9 Comparing Antiemetics table
Medication cards like this are intended to assist students to learn key points about each medication. Because information about medication is constantly changing, nurses should always consult evidence-based resources to review current recommendations before administering specific medication. Basic information related to each class of medication is outlined below.
Critical Thinking and Decision Making Questions
- A four year old is admitted for surgery. The child is very nauseated post-op. The order reads:
Promethazine 12.5-25mg PO/PR Q 4-6 hours PRN Is this a good choice for this client?
2. A patient is taking chemotherapy with a drug that has a high potential for causing nausea and vomiting. The nurse recognizes that the client will take a number of antiemetic medications. Which anti-emetics will be ordered to manage the nausea?
Note: Answers to the Clinical Reasoning Activities and Critical Thinking questions can be found in the Chapter 9: Gastrointestinal Medications Answer Key – Fundamentals of Nursing Pharmacology – 2nd Canadian Edition sections at the end of the book.
References
Bashashati, M. & McCallum, R. (2014). Neurochemical mechanisms and pharmacologic strategies in managing nausea and vomiting related to cyclic vomiting syndrome and other gastrointestinal disorders. European Journal of Pharmacology, 772, p 79. ↵
Brittin, T., Southard, B.T. & Al Khalili, Y. (2024). Promethazine. National Library of Medicine. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK544361/
Drug.com (2020-2025). Comparing dronabinol and nabilone. https://www.drugs.com/sfx/nabilone-side-effects.html
Flake, Z., Linn, B., & Hornecker, J. (2015). Practical selection of antiemetics in the ambulatory setting. American Family Physician, 91(5): pp 293-296. ↵
Griddine, A. and Bush, J. (2023, February). Ondansetron. National Library of Medicine. StatPearls. Ondansetron – StatPearls – NCBI Bookshelf
Ibrahim; M., Pellegrini; M., Preuss, C. (2024). Antiemetic Neurokinin-1 Receptor Blockers. National Library of Medicine. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK470394/
Isola, S., Hussain, A., Dua, A., Singh, K., Adams, N. (2023). Metoclopramide. National Library of Medicine. StatPearls. https://www.ncbi.nlm.nih.gov/books/NBK519517/
MedlinePlus [Internet]. Bethesda (MD): National Library of Medicine (US); [updated 2019 October 23]. Nausea and vomiting; [updated 2019 February 7; reviewed 2016 March 17; cited 2019 October 27]. https://medlineplus.gov/nauseaandvomiting.html. ↵
Mohr C, Jensen C, Padden N, Besel JM, Brant JM. (2021). Peppermint essential oil for nausea and vomiting in hospitalized patients: incorporating holistic patient decision making into the research design. Journal of Holistic Nursing, 39(2), 126-134. doi:10.1177/0898010120961579
Mohsenzadeh, A., Ahmadipour, S., Rahmani, P., Shakarami, P. (2018). Herbal remedies for the treatment of nausea and vomiting. Biomedical Research and Therapy, 5(5), 2252-2259. DOI:10.15419/bmrat.v5i5.437 https://doi.org/10.15419/bmrat.v5i5.437
Riad, M. & Hithe, C. (2023). Scopolamine. National Library of Medicine. StatPearls. Scopolamine – StatPearls – NCBI Bookshelf
Singh, K., Jain, A., Panchal, I., Madan, H., Gupta, A., Sharma, A., Gupta, S., Kostojchin, A., Singh, A., Sandhu, I., Mittal, J., Bhogal, L., Kolli, S., Bejugam, V., Chaturvedi, S., Bhalla, A., Piplani, S. (2023). Ondansetron-induced QT prolongation among various age groups: a systematic review and meta-analysis. Egypt Heart Journal, 75(56). doi: 10.1186/s43044-023-00385-y PMCID: PMC10317942 PMID: 37395900
Sealock, K. & Seneviratne, C. (2021). Lilley’s Pharmacology for Canadian Health Care Practice (4th ed.). Elsevier: Canada
Vallerand, A. & Sanoski, C. (2024). Davis’s Canadian drug guide for nurses (19th ed.). F.A. Davis Company: Canada
Media Attributions
- Figure 9.8a “Scopoderm 278:365” by Andreas Nilsson is licensed under CC BY-NC-ND 2.0 ↵
- Figure 9.8b “Metoclopramide” by John Campbell is licensed under CC0 ↵
- Figure 9.8c “Eichelbaum2.jpg” by Michel Eichelbaum is licensed under CC BY-SA 3.0 DE ↵
- Figure 9.8d”000817lg Zofran 8 MG Oral Tablet.jpg” by NLM is licensed under CC0 ↵
- Figure 9.8e “Ondansetron (1)” by M is licensed under CC BY-NC 2.0 ↵
- Figure 9.8f Steven-Johnson Syndrome rash. https://commons.wikimedia.org/wiki/File:Stevens-johnson-syndrome.jpg
- Figure 9.8g “Marinol – Dronabinol” by Steffen Geyer is licensed under CC BY-NC 2.0 &
- Figure 9.8h “Medical Marijuana” by Circe Denyer is licensed under CC0 ↵
- Figure 9.8i Ginger https://commons.wikimedia.org/wiki/File:Starr_070730-7818_Zingiber_officinale.jpg
- Figure 9.8j https://commons.wikimedia.org/wiki/File:Mentha_%C3%97_piperita%E2%80%93IMG_6075.jpg

