12.12 Aminoglycosides
Aminoglycosides are potent broad-spectrum antibiotics that are useful for treating severe infections. This class of antimicrobials treats severe staphylococcus infections when penicillins or other less toxic meds are contraindicated. It is often used in combination with other antibiotics due to synergistic effects.
Indications for Use:
Streptomycin is used for streptococcal endocarditis and a second line treatment for tuberculosis. Neomycin is used in the treatment of hepatic encephalopathy as adjunct therapy to lower ammonia levels and is also used as a bowel prep for colon procedures. it is also used for enterococcal infections such as urinary tract infections and pelvic inflammatory disease.
Mechanism of Action:
Aminoglycosides are bactericidal against gram-positive and gram-negative organisms. They bind with the area of the ribosome known as the 30S subunit, inhibiting protein synthesis in the cell wall and resulting in bacterial death (see Figure 12.12). Aminoglycosides may be given with beta-lactam medications to facilitate transport of aminoglycoside across the cellular membrane, resulting in a synergistic effect and increasing drug effectiveness. They are ineffective against anaerobic bacteria and have a narrow therapeutic index, meaning they require close monitoring due to potential kidney and ear toxicity.
Nursing Considerations:
Administration: Many aminoglycosides are poorly absorbed in the GI tract; therefore, the majority are given IV or IM. Neomycin is given orally for hepatic encephalopathy.
Ensure client is well-hydrated with 1500-2000 mL/day during therapy.
Aminoglycosides are potentially nephrotoxic, ototoxic and neurotoxic. They should be administered cautiously. Blood peak and trough levels should be performed to titrate a safe dose for each client. Ensure to assess and report any changes indicating early toxicity.
Pediatrics: Safe to use in pediatric clients, with dose adjustments made based on the client’s weight.
Pregnancy: Some aminoglycosides are not safe for use in pregnancy, as they can cause fetal harm.
Older adult: monitor renal function and dosages will likely be reduced.
Monitoring:
- Assess the following labs prior to therapy: renal function and liver function.
- **Close monitoring due to risk of nephrotoxic (damaging to kidney; renal tubular toxicity reducing blood flow to the kidneys), neurotoxic (damaging to the nervous system), and ototoxic (damaging to the ear; auditory impairment and vestibular [8th cranial nerve] impairment).
- Peak and trough levels are used to titrate this medication to a safe dose.
- Assess for signs of decreased renal function such as declining urine output and increasing blood urea nitrogen (BUN), creatinine, and declining glomerular filtration rate (GFR).
- Assess for damage to the neurological system such as increasing peripheral numbness or tingling in the extremities.
- Assess for hearing loss or hearing changes throughout the course of drug administration.
Side /Adverse Effects
Common effects include headache and nausea.
Signs of ototoxicity include dizziness, vertigo and tinnitus.
Signs of nephrotoxicity – elevated GFR. Usually reversible. Higher risk if client pregnant, hepatic dysfunction or dehydrated. Concurrent use of NSAIDs, cyclosporine, and diuretics increase risk.
Risk of neuromuscular blockade, includes muscle weakness or paralysis. Do not give med if they have myasthenia gravis.
Allergic reactions are rare.
(Chaves & Tadi, 2023)
Drug Interactions
- Loop diuretics: increased risk of ototoxicity.
- Oral anticoagulants: neomycin increases the effects of warfarin, assess for bleeding.
Client Teaching:
- Monitor for signs of hypersensitivity and auditory changes. This may include tinnitus and hearing loss.
- Report any issues with muscle weakness.
- Avoid taking NSAIDs and ensure to stay well-hydrated.
- Clients may also experience accompanying vertigo while on the medication.
- Drink plenty of fluids while taking the medication.
- Female clients should notify their provider if pregnancy is planned or if they are actively breastfeeding Unbound Medicine, n.d.)
Streptomycin and Gentamycin Medication Card
Now let’s take a closer look at the medication card for streptomycin and gentamycin (Daily Med 2019; UpToDate, 2021). Because information about medication is constantly changing, nurses should always consult evidence-based resources to review current recommendations before administering specific medication.
To help with comparing the medications and to learn important considerations for each medication, refer to the Chapter 12 Antimicrobials Medication Cards
Medication Card: Aminoglycosides
Prototypes: streptomycin, gentamicin
Mechanism: Bactericidal, gram – and some gram + organisms. Exact mechanism not fully known, similar to tetracyclines. Very potent. Resistance to med can be overcome if used with penicillin or vancomycin. Inactivated by lactams (penicillin & cephalosporins) when coadministered to pts with renal insufficiency.
Indications
- Serious Gram+ infections
- Enterococcus infections: GI, GU
- Streptococcal Endocarditis, Respiratory infections
- Second line treatment for TB
- Neomycin is used int he treatment for hepatic encephalopathy
Administration
- Routes: IM, IV, topical
- never PO: poor absorption
- given w/B-lactams, vanco for synergy
Side Effects
- Ototoxicity (more common with pts taking furosemide)
- Nephrotoxicity. Risk increases if dehydrated, pregnant or with hepatic dysfunction.
- 8th cranial nerve damage = dizziness, nystagmus, vertigo, ataxia, tinnitus, roaring in ears, hearing impairment
- GI upset
- Rash
- Risk for severe neurotoxic reactions, especially with renal impairment. Can result in respiratory paralysis if given soon after anesthesia or muscle relaxant
- Can cause harm to fetus and breastfed infants
Contraindications
- Preg/nursing: congenital deafness
- Allergy to med
- Renal impairment
- Loop diuretics
- Oral anticoagulants
Nursing Considerations
- SEs most likely if pt: has hx of renal impairment, is dehydrated, getting high dosage, prolonged therapy, using other ototoxic drugs
- Renal assessment: proteinuria, BUN, creatinine
- Neuro assessment
- Hearing can come back after drug tx
- Report diarrhea immediately
Clinical Reasoning and Decision-Making Activity
Using the above grid information, consider the following clinical scenario question:
A client is admitted with streptococcal endocarditis and the nurse is preparing the morning dose of streptomycin. The lab test has not yet arrived to obtain the trough level, and the drug is now overdue to be given. What is the nurse’s next best response?
Note: Answers to the Clinical Reasoning Activities and Critical Thinking questions can be found in the Chapter 12: Antimicrobial Medications answer key – Fundamentals of Nursing Pharmacology – 2nd Canadian Edition section at the end of the book.
Image Description
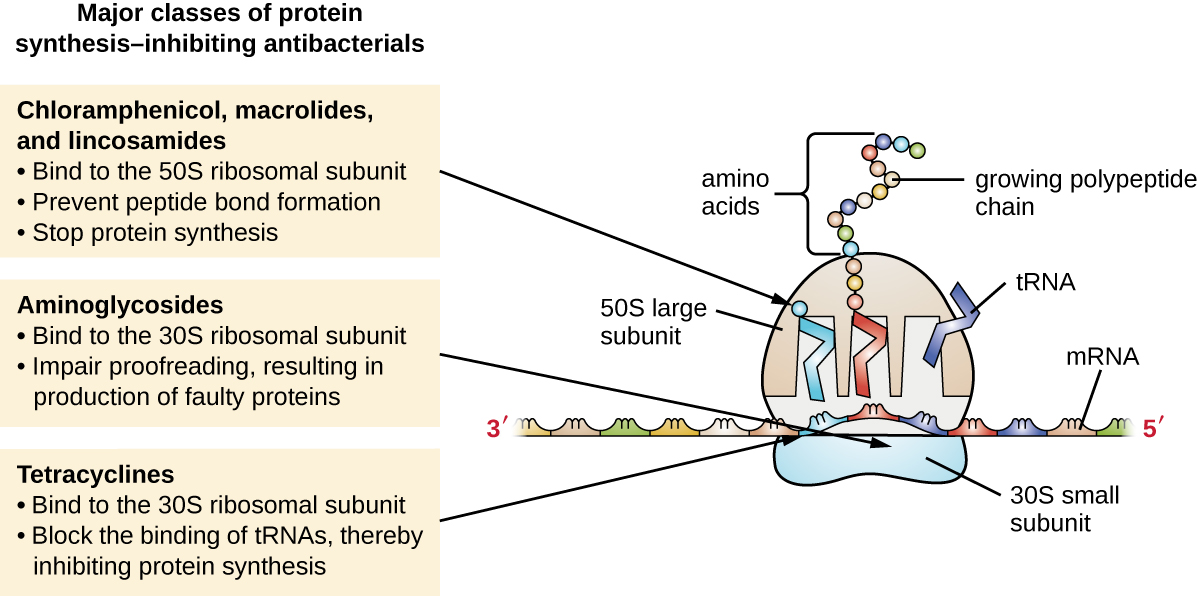
Figure 3.13 Medications that inhibit protein synthesis: Diagram of a cell undergoing protein synthesis that describes the major classes of protein synthesis–inhibiting antibacterials. These include:
- Chloramphenicol, macrolides, and lincosamides, which:
- Bind to the 50S ribosomal subunit
- Prevent peptide bond formation
- Stop protein synthesis
- Aminoglycosides, which:
- Bind to the 30S ribosomal subunit
- Impair proofreading, resulting in production of faulty proteins
- Tetracyclines, which:
- Bind to the 30S ribosomal subunit
- Block the binding of tRNAs, thereby inhibiting protein synthesis
References
Chades, B. & Tadi, P. (2023). Gentamycin. National Library of Medicine. StatPearls [Internet]. https://www.ncbi.nlm.nih.gov/books/NBK557550/
Daily Med, https://dailymed.nlm.nih.gov/dailymed/index.cfm, used for hyperlinked medications in this module. Retrieved June 27, 2019 ↵
OpenStax (2026). This work is a derivative of Microbiology by OpenStax licensed under CC BY 4.0. Access for free at https://openstax.org/books/microbiology/pages/1-introduction ↵
uCentral from Unbound Medicine. https://www.unboundmedicine.com/ucentral ↵
UpToDate (2021). Streptomycin. https://www.uptodate.com/contents/search ↵

