10.4 Thyroid Medications V2
To understand the purpose of thyroid medications and how they work in the body, this unit will begin with:
- a review of physiology of the thyroid gland including its function, regulation and the release of thyroid hormones.
- an overview of disorders of thyroid gland including iodine deficiency, hypothyroidism, and hyperthyroidism.
- a review of the physiology of the parathyroid glands
- an overview of disorders of the parathyroid gland, hyperparathyroidism and hypoparathyroidism.
Medications that will be examined are:
- hypothyroidism: levothyroxine
- antithyroid medication: propylthiouracil (PTU)
- osteoporosis medications:
- calcitonin
- bone reabsorption inhibitor: alendronate
Thyroid Basics: A&P Review
The thyroid is a butterfly-shaped organ located anterior to the trachea, just inferior to the larynx (see Figure 10.4a).[1] Each of the thyroid lobes is embedded with parathyroid glands.

Synthesis and Release of Thyroid Hormones
Thyroid hormone production is dependent on the hormone’s essential component: iodine. T3 and T4 hormones are produced when iodine attaches to a glycoprotein called thyroglobulin. The following steps outline the hormone’s assembly: Binding of TSH to thyroid receptors causes the cells to actively transport iodide ions across their cell membrane from the bloodstream. As a result, the concentration of iodide ions “trapped” in the thyroid cells is many times higher than the concentration in the bloodstream. The iodide ions undergo oxidation (i.e., their negatively charged electrons are removed) and enzymes link the iodine to tyrosine to produce triiodothyronine (T3), a thyroid hormone with three iodines, or thyroxine (T4), a thyroid hormone with four iodines. These hormones remain in the thyroid follicles until TSH stimulates the release of free T3 and T4 into the bloodstream. In the bloodstream, less than one percent of the circulating T3 and T4 remains unbound. This free T3 and T4 can cross the lipid bilayer of cell membranes and be taken up by cells. The remaining 99 percent of circulating T3 and T4 is bound to specialized transport proteins called thyroxine-binding globulins (TBGs), to albumin, or to other plasma proteins. This “packaging” prevents their free diffusion into body cells. When blood levels of T3 and T4 begin to decline, bound T3 and T4 are released from these plasma proteins and readily cross the membrane of target cells. T3 is more potent than T4, and many cells convert T4 to T3 through the removal of an iodine atom.
Regulation of Thyroid Hormone Synthesis
A negative feedback loop controls the regulation of thyroid hormone levels. As shown in Figure 9.6b,[2] low blood levels of T3 and T4 stimulate the release of thyrotropin-releasing hormone (TRH) from the hypothalamus, which triggers secretion of TSH from the anterior pituitary. In turn, TSH stimulates the thyroid gland to secrete T3 and T4. The levels of TRH, TSH, T3, and T4 are regulated by a negative feedback system in which increasing levels of T3 and T4 decrease the production and secretion of TSH.

Functions of Thyroid Hormones
The thyroid hormones T3 and T4 are often referred to as metabolic hormones because their levels influence the body’s basal metabolic rate, which is the amount of energy used by the body at rest. When T3 and T4 bind to intracellular receptors located on the mitochondria, they cause an increase in nutrient breakdown and the use of oxygen to produce ATP. In addition, T3 and T4 initiate the transcription of genes involved in glucose oxidation. Although these mechanisms prompt cells to produce more ATP, the process is inefficient, and an abnormally increased level of heat is released as a byproduct of these reactions. This calorigenic effect (calor- = “heat”) raises body temperature.
Adequate levels of thyroid hormones are also required for protein synthesis and for fetal and childhood tissue development and growth. They are especially critical for normal development of the nervous system both in utero and in early childhood, and they continue to support neurological function in adults. Thyroid hormones also have a complex interrelationship with reproductive hormones, and deficiencies can influence libido, fertility, and other aspects of reproductive function. Finally, thyroid hormones increase the body’s sensitivity to catecholamines (epinephrine and norepinephrine) from the adrenal medulla by upregulation of receptors in the blood vessels. When levels of T3 and T4 hormones are excessive, this effect accelerates the heart rate, strengthens the heartbeat, and increases blood pressure. Because thyroid hormones regulate metabolism, heat production, protein synthesis, and many other body functions, thyroid disorders can have severe and widespread consequences.
Disorders of the Thyroid Gland: Iodine Deficiency, Hypothyroidism, and Hyperthyroidism
As discussed above, dietary iodine is required for the synthesis of T3 and T4. For much of the world’s population, foods do not provide adequate levels of iodine because the amount varies according to the level in the soil in which the food was grown, as well as the irrigation and fertilizers used. Marine fish and shrimp tend to have high levels because they concentrate iodine from seawater, but many people in landlocked regions lack access to seafood. Thus, the primary source of dietary iodine in many countries is iodized salt. Fortification of salt with iodine became mandatory in Canada in 1949, and international efforts to iodize salt in the world’s poorest nations continue today.
Iodine deficiency
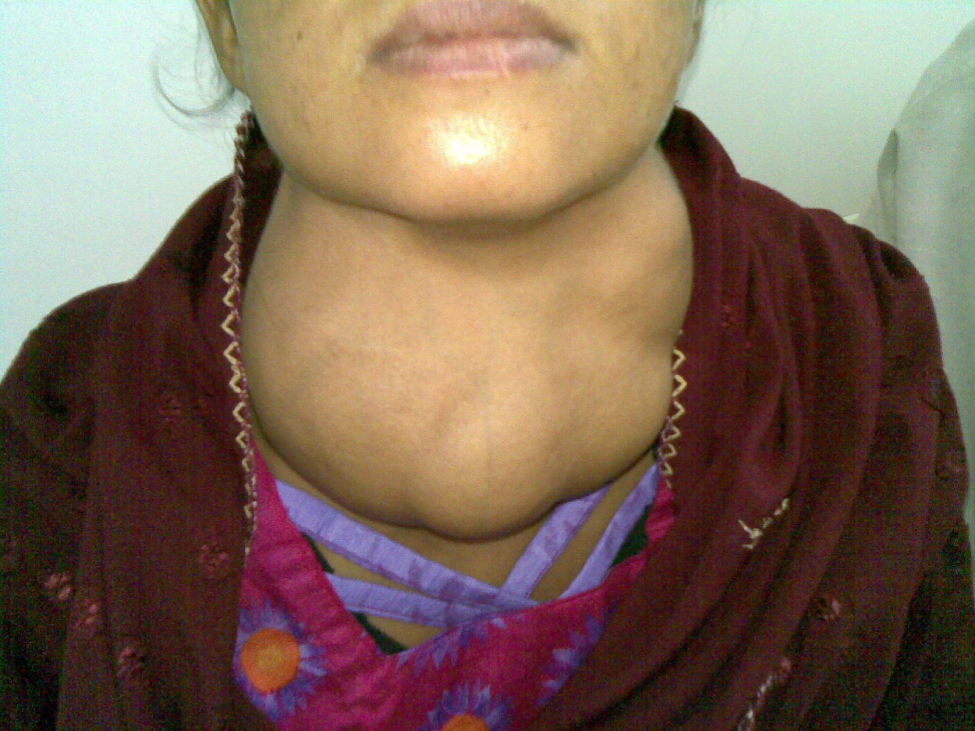
Dietary iodine deficiency can result in the impaired ability to synthesize T3 and T4, leading to a variety of severe disorders. When T3 and T4 cannot be produced, TSH is secreted in increasing amounts. As a result of this hyperstimulation, thyroglobulin and colloid accumulate in the thyroid gland and increase the overall size of the thyroid gland, a condition called a goiter (see Figure 10.4b). A goiter is only a visible indication of the deficiency. Other disorders related to iodine deficiency include impaired growth and development, decreased fertility, and prenatal and infant death. Moreover, iodine deficiency is the primary cause of preventable mental retardation worldwide. Neonatal hypothyroidism (cretinism) is characterized by cognitive deficits, short stature, and sometimes deafness and muteness in children and adults born to mothers who were iodine-deficient during pregnancy.
Hypothyroidism
In areas of the world with access to iodized salt, dietary deficiency is rare. Instead, inflammation of the thyroid gland is a common cause of hypothyroidism or low blood levels of thyroid hormones. Hypothyroidism is a disorder characterized by a low metabolic rate, weight gain, cold extremities, constipation, reduced libido, menstrual irregularities, and reduced mental activity, and requires long-term thyroid hormone replacement therapy.
Hyperthyroidism
Hyperthyroidism is an abnormally elevated blood level of thyroid hormones. It is often caused by a pituitary or thyroid tumor. In Graves’ disease, the hyperthyroid state results from an autoimmune reaction in which antibodies overstimulate the follicle cells of the thyroid gland. Hyperthyroidism can lead to an increased metabolic rate, excessive body heat and sweating, diarrhea, weight loss, tremors, and increased heart rate. The person’s eyes may bulge (called exophthalmos) as antibodies produce inflammation in the soft tissues of the orbits. The person may also develop a goiter.
Hyperthyroidism is often treated by thyroid surgery or with radioactive iodine (RAI) therapy. Clients are asked to follow radiation precautions after RAI treatment to limit radiation exposure to others, especially pregnant women and young children, such as sleeping in a separate bed and flushing the toilet 2-3 times after use. The RAI treatment may take up to several months to have its effect. The end result of thyroid surgery or RAI treatment is often hypothyroidism, which is treated by thyroid hormone replacement therapy.[3]
Calcitonin
The thyroid gland also secretes another hormone called calcitonin. Calcitonin is released in response to elevated blood calcium levels. It decreases blood calcium concentrations by:
- Inhibiting the activity of osteoclasts (bone cells that breakdown bone matrix and release calcium into the circulation)
- Decreasing calcium absorption in the intestines
- Increasing calcium loss in the urine
Pharmaceutical preparations of calcitonin are prescribed to reduce osteoclast activity in people with osteoporosis. Osteoporosis is a disease that can be caused by glucocorticoids.
Calcium is critical for many other biological processes. It is a second messenger in many signaling pathways and is essential for muscle contraction, nerve impulse transmission, and blood clotting. Given these roles, it is not surprising that blood calcium levels are tightly regulated by the endocrine system. The parathyroid glands are primarily involved in calcium regulation.
Calcium Regulation: Parathyroid Glands
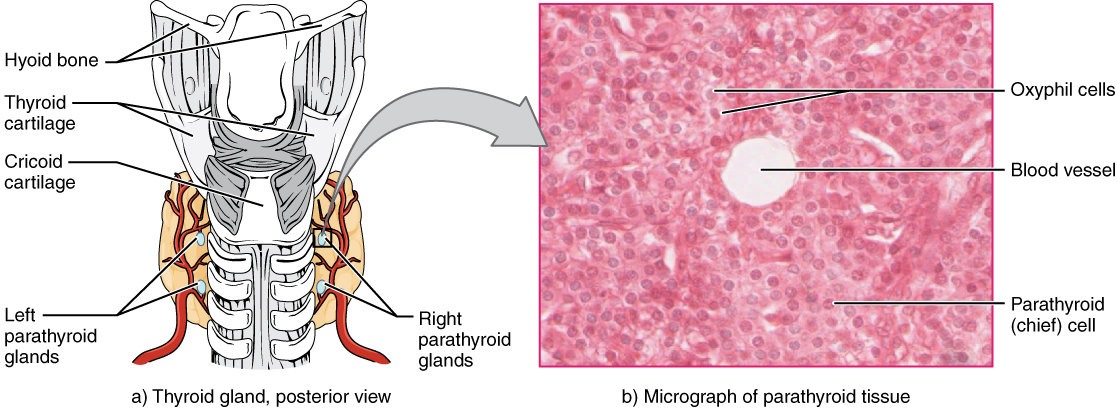
The parathyroid glands are four tiny, round structures usually embedded in the posterior surface of the thyroid gland (see Figure 10.4d).[4] The primary function of the parathyroid glands is to regulate blood calcium levels by producing and secreting parathyroid hormone (PTH) in response to low blood calcium levels.
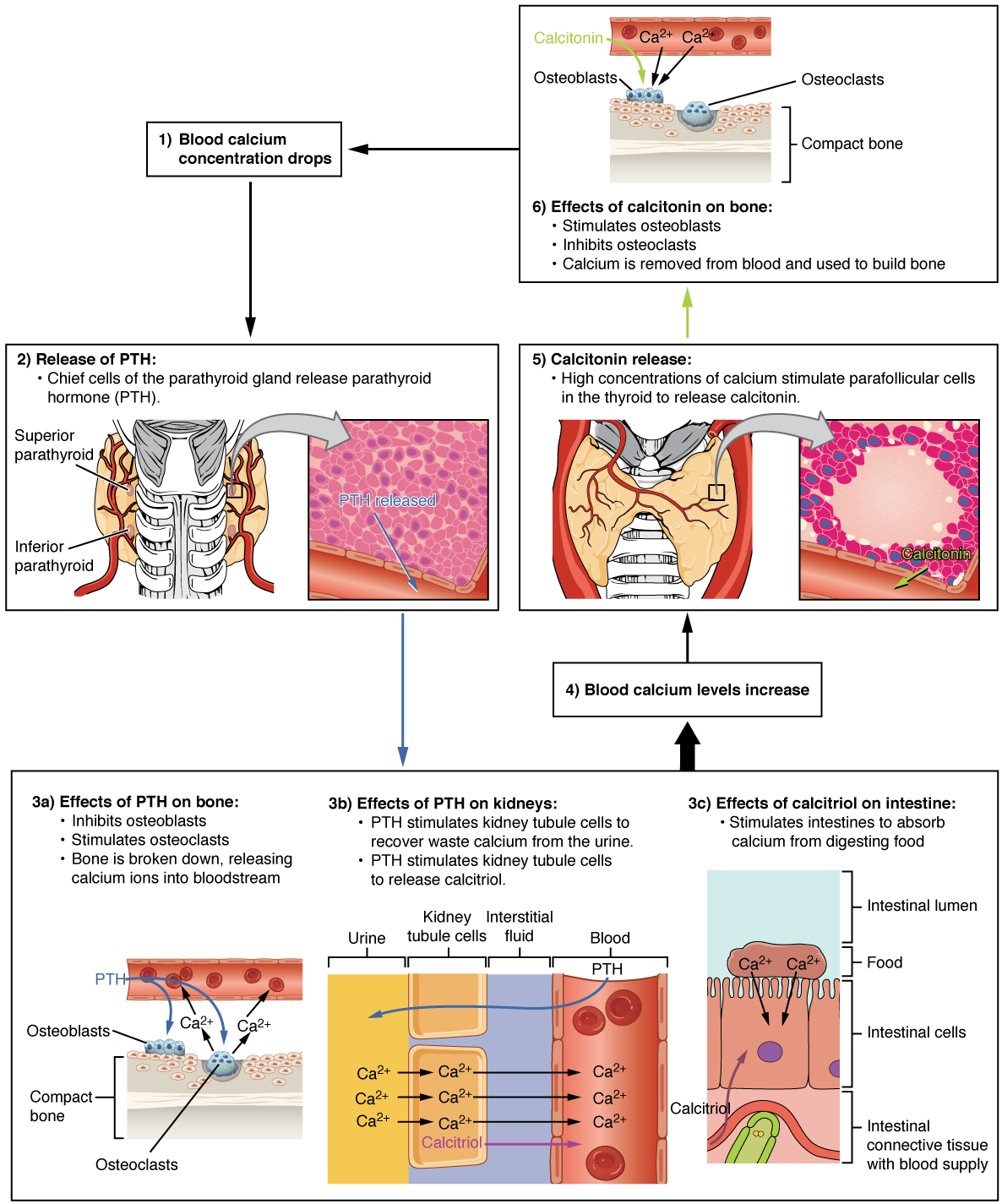
PTH secretion causes the release of calcium from the bones by stimulating osteoclasts that degrade bone and then release calcium into the bloodstream. PTH also inhibits osteoblasts, the cells involved in bone deposition, thereby keeping calcium in the blood. PTH also causes increased reabsorption of calcium (and magnesium) in the kidney and initiates the production of the steroid hormone calcitriol, which is the active form of vitamin D3. Calcitriol then stimulates increased absorption of dietary calcium by the intestines. A negative feedback loop regulates the levels of PTH, with rising blood calcium levels inhibiting further release of PTH. (See Figure 10.4e for an illustration of the role of parathyroid hormone in maintaining blood calcium homeostasis.)[5]
Disorders of the Parathyroid Glands
Abnormally high activity of the parathyroid gland can cause hyperparathyroidism, a disorder caused by an overproduction of PTH that results in excessive degradation of bone and elevated blood levels of calcium, also called hypercalcemia. Hyperparathyroidism can thus significantly decrease bone density, which can lead to spontaneous fractures or deformities. As blood calcium levels rise, cell membrane permeability to sodium is also decreased, and thus the responsiveness of the nervous system is reduced. At the same time, calcium deposits may collect in the body’s tissues and organs, impairing their functioning.
In contrast, abnormally low blood calcium levels may be caused by parathyroid hormone deficiency, called hypoparathyroidism, which may develop following injury or surgery involving the thyroid gland. Low blood calcium increases membrane permeability to sodium, thus increasing the responsiveness of the nervous system, resulting in muscle twitching, cramping, spasms, or convulsions. Severe deficits can paralyze muscles, including those involved in breathing, and can be fatal.
Endocrine Gland Medications
In this section, we will examine three different types of thyroid medications. This includes medications for hypothyroidism (levothyroxine), for hyperthyroidism (Propylthiouracil or PTU), and two osteoporosis medications, calcitonin and alendronate.
Levothyroxine
Levothyroxine is a thyroid replacement drug used to treat hypothyroidism. It is used to treat primary, secondary and tertiary hypothyroidism. Primary is when there is a problem with the thyroid gland, secondary is then there is a problem with the pituitary gland and tertiary is sporadic (Eghtedari & Correa, 2023)
Mechanism of Action
Oral levothyroxine sodium is a synthetic T4 hormone that exerts the same physiologic effect as endogenous T4, thereby maintaining normal T4 levels when a deficiency is present.
Nursing Considerations
Administration: oral, comes in many forms such as capsule, solution, and tablets. Intravenous route also available.
- Administer 30-60 minutes before breakfast or 3-4 hours after dinner. Gastric acidity is needed for absorption.
- Do not give with foods contained calcium or iron
- Tablet: take on an empty stomach with a full glass of water
- Capsules: do no crush or cut, swallow whole.
- Avoid taking levothyroxine with soybean, papaya and grapefruit as absorption can be impaired.
No dose adjustments with hepatic or renal disease.
Pregnancy: monitor TSH levels and may need to increase levothyroxine requirements (Daily Med, 2026).
Drug interactions:
- Do not give with antacids or proton pump inhibitors as they can decrease absorption.
- Calcium carbonate and iron bind to levothyroxine and reduce the absorption.
- Give 4 hours apart from bile acid sequestrants (e.g., colesevelam) as they reduce levothyroxine absorption.
- Levothyroxine increases the response to oral anticoagulant therapy. Therefore, a decrease in the dose of anticoagulant may be warranted with correction of the hypothyroid state or when the levothyroxine dose is increased. Closely monitor INR results and anticipate dosage adjustments.
Assessment
- Narrow therapeutic window so closely monitored with TSH levels. Assess TSH levels before and then 4-6 weeks after starting the med. Once at therapeutic levels, monitor every 4-6 months, and then yearly (Eghtedari & Correa, 2023).
- Monitor pulse and blood pressure prior to therapy and regularly.
Contraindicated with hyperthyroidism and adrenal insufficiency.
Diabetic clients: may worsen glycemic control. Clients may need a higher dosage of antidiabetic medications. Carefully monitor glycemic control, especially when thyroid therapy is started, changed, or discontinued
Adverse/Side Effects
Due to narrow therapeutic window, there is a risk of under or over dosage. Adverse effects affect most body systems, including growth and development, cardiovascular function, bone metabolism, reproductive function, cognitive function, emotional state, GI function and glucose and lipid metabolism (Drug Bank, 2026).
Adverse effects that result from excessive dosing can result in a hyperthyroid-like presentation, particularly increased heart rate, cardiac wall thickness, and cardiac contractility that may precipitate angina or arrhythmias, particularly in clients with cardiovascular disease and in elderly clients. Levothyroxine should be started at lower doses. If cardiac symptoms develop or worsen, hold the dose and contact the health care provider. Anticipate a lower dose prescribed or the medication to be withheld for one week then restarted at a lower dose.
Adverse effects can include:
- CV effects: angina, palpitations, myocardial infarction, atrial fibrillation.
- Neuro: insomnia, anxiety
- GI: weight loss, diarrhea, fatigue
- Integument: rash, alopecia, diaphoresis
- Endocrine: goiter, menstrual irregularities, heat intolerance, decreased bone density
- Elevated liver enzymes
Report any adverse effects as dosage adjustment may be warranted. Signs of overdose or over-medicated with elevated levels of thyroid hormone, can cause cardiac dysrhythmias. Immediately report any symptoms of tachycardia, chest pain, or palpitations to the provider. In the event of overdose or elevated TSH levels, hold the next dose and potentially for 2-6 days.
Client Teaching
- Clients should take thyroid replacement medications at the same time each day. If a dose is missed, take as soon as possible, unless already the next day.
- Notify the prescriber if more than 2-3 doses are missed.
- Clients should be aware that thyroid replacement medications do not cure hypothyroidism and therapy is lifelong.
- Clients should notify their healthcare provider if they experience signs of headache, diarrhea, sweating, increased heart rate, palpitations, or heat intolerance.
- Medications should be spaced four hours apart from medications like antacid, iron, or calcium supplements.
- Clients will be followed closely by their healthcare provider regarding their response to medication therapy and serum thyroid levels will be taken (Vallerand & Sanoski, 2024).
Example in Practice
A 35 year old client visits her nurse practitioner as she has been experiencing unusual fatigue, an intolerance to cold and weight gain. She says she exercises and eats well. She wakes up in the morning tired. Her BP is 105/65 mmHg, heart rate 55 bpm, RR 12 breaths/min and afebrile. The NP orders lab work: thyroid panel (TSH, T3 and T4), ferritin and CBC, fasting blood sugar, A1C and renal panel. The results come back that she has low TSH with the rest of her labs within normal limits. The client is ordered levothyroxine 112 mcg once a day. Teaching is provided on how to take the med correctly, precautions and adverse effects. The client is able to teach back to the nurse that she needs to take the med 30-60 minutes prior to breakfast. She knows to avoid juices such as grapefruit juice and to not take antacids or calcium supplements at the same time as taking the med. She will let the NP know if she plans to get pregnant. Lastly, she is able to verbalize possible side effects and knows which ones to report right away. She knows she will be on thyroxine for the rest of her life and is looking forward to feeling better.
Antithyroid Medication: Propylthiouracil (PTU)
Propylthiouracil (PTU) is an antithyroid medication used to treat hyperthyroidism or to ameliorate symptoms of hyperthyroidism in preparation for thyroidectomy or radioactive iodine therapy.
Mechanism of Action
Propylthiouracil inhibits the synthesis of thyroid hormones.
Nursing Considerations
Administration: oral administration. The total daily dosage is usually given in 3 equal doses at approximately 8-hour intervals. Propylthiouracil can cause hypothyroidism necessitating routine monitoring of TSH and free T4 levels, with adjustments in dosing to maintain a euthyroid state.
Pregnancy: Propylthiouracil crosses the placenta and can cause fetal liver failure, goiter, and cretinism if administered to a pregnant woman.
Adverse/side effects:
Liver injury resulting in liver failure, liver transplantation, or death has been reported. Clients should be instructed to report any symptoms of hepatic dysfunction (anorexia, pruritus, and right upper quadrant pain), particularly in the first six months of therapy.
Agranulocytosis is a potentially life-threatening side effect of propylthiouracil therapy. Agranulocytosis typically occurs within the first 3 months of therapy. Clients should be instructed to immediately report any symptoms suggestive of agranulocytosis, such as fever or sore throat.
Cases of vasculitis resulting in severe complications and death have been reported in clients receiving propylthiouracil therapy. If vasculitis is suspected, discontinue therapy and initiate appropriate intervention.
Client Teaching
- Clients should take the medication as directed at regular dosing intervals.
- They should monitor their weight 2-3 times per week.
- Clients should be advised that medications may cause drowsiness, and they should report any signs of sore throat, fever, headache, jaundice, bleeding, or bruising.
Osteoporosis Medication: Calcitonin
Calcitonin is used to treat osteoporosis in post-menopausal women, particularly if they are in the post-menopausal phase for a minimum of five years. It is also used as a secondary treatment option for Paget disease of the bone. It can provide relief from bone pain, reverse neurological deficits, reduce blood flow to the diseased bone, and may even improve hearing loss that is associated with Paget disease (McLaughlin, Awosika & Jialal, 2023).
Mechanism of Action
Calcitonin is a calcitonin receptor agonist. Calcitonin is released by the thyroid gland. It acts primarily on bone and also has effects on the kidneys and the gastrointestinal tract. Calcitonin inhibits osteoclasts, resulting in lower bone mineral density (BMD) losses and the risk of osteoporotic fractures can be lowered. Calcitonin also exerts its effects on tubular epithelium of the kidneys, inducing diuresis and decreases reabsorption, which results in reduced serum calcium and phosphate levels (McLaughlin, Awosika & Jialal, 2023).
In summary: when calcium levels are too high, the thyroid gland secretes more calcitonin. This decreases the osteoclasts activity and causes the kidney to excrete more calcium. If the osteoclast activity is decreased, the osteoblasts still continue to work building up bone matrix, resulting in stronger bones. If we give calcitonin to prevent osteoporosis, then calcium is taken from the blood and used by osteoblasts to improve the bone matrix.
Note: Osteoclasts consume bone matrix by taking calcium from the bone and putting it into the blood to maintain serum calcium levels. Osteoblasts build up bone matrix by taking calcium from the blood to create more bone matrix.
Nursing Considerations
Administration: nasal spray with one spray in one side of the nose daily, alternating nostrils. See Figure 10.4g for an image of calcitonin nasal spray.
The nasal spray pump should be primed before the first administration.
Unopened calcitonin can be stored in the refrigerator until opened, but should not be refrigerated between doses. Opened bottles stored at room temperature should be discarded after 30 days of initial dose.
Pregnancy: Calcitonin should not be used during pregnancy.
Caution with clients with bipolar disorder and taking lithium. It can potentially lower lithium levels (McLaughlin, Awosika & Jialal, 2023).
Adverse/Side Effects:
Adverse effects include serious hypersensitivity reactions (bronchospasm, swelling of the tongue or throat, anaphylaxis and anaphylactic shock), hypocalcaemia, nasal mucosa adverse events, and malignancy.
Client Teaching
- Clients should be advised to take medications as directed.
- They should report any signs of hypercalcemia or an allergic response.
- Ensure clients are taught how to administer correctly.
- Advise clients that they may experience flushing and warmth following injection.
- Post-menopausal women should adhere to a diet high in calcium and vitamin D, and should be educated regarding the importance of exercise for reversing bone loss.

Bone Reabsorption Inhibitor: Alendronate
Alendronate is a Bisphosphonate, used for the prevention and treatment of osteoporosis in postmenopausal women, to increase bone mass in men with osteoporosis, and for glucocorticoid-induced osteoporosis (Vallerand & Sanoski, 2024).
Mechanism of Action
Alendronate is a bisphosphonate that inhibits osteoclast-mediated bone resorption. By preventing the breakdown of bone and enhancing the formation of new bone, alendronate assists in reversing bone loss and decreases the risk of fractures.
Nursing Considerations
Administration: oral formulations. May be ordered once a day or weekly. Tablet or effervescent tablets
- Alendronate should be taken upon arising for the day, but should be administered at least one-half hour before the first food, beverage, or medication of the day with plain water only. Other beverages (including mineral water), food, and some medications are likely to reduce the absorption of alendronate.
- Effervescent tablets: dissolve in 125 mL of plain water, wait 5 minutes, stir for 10 seconds, then drink.
- Clients should not lie down for at least 30 minutes and until after their first food of the day.
- Clients may also require calcium and vitamin D supplementation, especially if concurrently taking glucocorticoids.
Pre-treatment Assessment and Monitoring:
- Assess bone mass before and periodically during therapy
- Assess for symptoms of Paget’s disease (bone pain, headache, decreased visual or auditory acuity)
- Labs: serum calcium, vitamin D levels
Pregnancy: do not take if pregnant as it may cause fetal harm.
Contraindicated with clients with kidney disease with creatinine clearance less than 35 mL/min.
Contraindicated in the following conditions: hypocalcaemia, preexisting vitamin D deficiency, the inability to sit or stand for 30 minutes after swallowing, esophageal abnormalities that delay emptying, and clients at risk for aspiration.
Adverse/Side Effects:
Discontinue alendronate if severe musculoskeletal pain occurs. A bone mineral density measurement should be made at the initiation of therapy and repeated after 6 to 12 months of combined alendronate and glucocorticoid treatment.
Client Teaching
- Clients should take medication as directed at the same time each day, first thing in the morning. Only take with 250 mL of plain water. Do not double doses if a dose is missed.
- Clients should remain upright after they take medication for 30 minutes to minimize stomach and esophageal irritation.
- Clients should eat a balanced diet and may seek advice from the healthcare provider regarding supplementation with calcium and vitamin D.
- Clients should participate in regular exercise to help increase bone strength.
- Use sunscreen to protect against photosensitivity
Vallerand & Sanoski, 2024
Medication Card Comparing Thyroid (levothyroxine, propylthiouracil) and Osteoporosis Medications (calcitonin, alendronate).
Now let’s take a closer look at the Chapter 10 Endocrine System Thyroid Medications 2026 This table is intended to assist students to learn key points about each medication. Because information about medication is constantly changing, nurses should always consult evidence-based resources to review current recommendations before administering specific medication. Basic information related to each class of medication is outlined below.
| Class/ Medication | Therapeutic Effects | Administration Considerations | Adverse/Side Effects and Contraindications |
| Thyroid replacement
levothyroxine |
Increases T4 levels in hypothyroidism | Take with a full glass of water as tablet may rapidly disintegrate
Administer levothyroxine as a single daily dose, on an empty stomach, one-half to one hour before breakfast Administer at least 4 hours before or after drugs known to interfere with levothyroxine absorption Anticipate lower dosages in elderly clients with pre-existing cardiac disease Assess TSH levels before and then 4-6 weeks after starting the med. Once at therapeutic levels, monitor every 4-6 months, and then yearly |
Many potential adverse effects, including cardiac, neuro, GI, and endocrine effects.
CV: palpitations, angina, dysrhythmias Neuro: anxiety, insomnia GI: nausea, diarrhea, weight loss Integ: alopecia, Endocrine: menstrual irreg., decr bone density
Hypersensitivity reactions Drug interactions: PPI, antacids and bile acid sequestrants will decrease absorption. Take 4 hours apart from levothyroxine. Anticoagulants with Levothyroxine: increases anticoagulant effects. Dose adjustment needed. Narrow therapeutic window so closely monitored with TSH levels. Diabetic clients: may worsen glycemic control, adjust dosing.
|
| Antithyroid
propylthiouracil (PTU) |
Inhibit production of T4 to treat hyperthyroidism
|
Usually administered every 8 hours
May cause hypothyroidism so TSH and T4 levels should be monitored |
Risk of Hypothyroidism, monitor TSH levels
Risk of liver injury. agranulocytosis Vasculitis Do not take if pregnant: risk of fetal harm |
| Calcium regulator
calcitonin |
Treats osteoporosis
Used for post-menopausal women, 5 years post menopause Secondary treatment of Paget’s disease
|
Administer nasal spray with one spray in one side of the nose daily
Discard unrefrigerated bottle after 30 days of opening May store unopened bottles in refrigerator until expiration date |
Serious hypersensitivity reactions (bronchospasm, swelling of the tongue or throat, anaphylaxis, and anaphylactic shock)
Hypocalcemia Nasal mucosa irritation Malignancy Contraindicated during pregnancy Caution if client on lithium, may lower lithium levels |
| Bisphosphonates
alendronate |
Enhances bone mineral density in osteoporosis
prevention and treatment of osteoporosis in postmenopausal women, and for glucocorticoid-induced osteoporosis |
Administered upon arising and at least one-half hour before the first food or drink or other meds.
Take with plain water only sit or stand for 30 minutes after administration Concurrent calcium and vitamin D supplements may be required Assess bone mass before and periodically during therapy |
Adverse effects include: upper GI tract, severe musculoskeletal pain
Risk of osteonecrosis of the jaw Contraindicated in pregnancy, hypocalcaemia, and kidney disease |
Critical Thinking and Decision-Making Learning Activities
- A client has type 1 diabetes and has recently been diagnosed with hypothyroidism. The client has been provided some teaching on how to take levothyroxine (Synthroid) and other important considerations. The client states, “I am glad I will need a much lower dose of insulin now that I am on thyroxine.” Does the client need more health teaching?
- A post-menopausal women has osteoporosis and the prescriber is concerned with the risk for fractures if the client fell. They are prescribed calcitonin. What are some concerns while taking this med?
Note: Answers to the Clinical Reasoning Activities and Critical Thinking questions can be found in the Chapter 10: Endocrine System Medications: Part 1 Answer Key – Fundamentals of Nursing Pharmacology – 2nd Canadian Edition section at the end of the book.
Image Descriptions
Figure 9.6b Negative Feedback Loop: A flowchart demonstrating the negative feedback loop regulating thyroid hormone levels. It details the following steps:
- Metabolic rate and/or T3 and T4 concentration in blood:
- High? Hypothalamus stops TRH release. Anterior pituitary stops TSH release.
- Low? Hypothalamus releases TRH. This triggers TSH release by the pituitary.
- Effects of TSH release: Triggers release of T3 and T4 by thyroid follicle cells.
- Effects of T3 and T4 release:
- Increased basal metabolic rate of body cells.
- Rise in body temperature (calorigenic effect).
- Negative feedback:
- Elevated T3 and T4 levels inhibit release of TRH and TSH.
- If T3 and T4 are high:
- Hypothalamus stops TRH release.
- Anterior pituitary stops TSH release.
Figure 9.6e Parathyroid Hormone in Maintaining Blood Calcium Homeostasis: A flowchart demonstrating how parathyroid hormone (PTH) helps to maintain blood calcium homeostasis. It details the following steps:
- Blood calcium concentration drops.
- Release of PTH: chief cells of the parathyroid gland release parathyroid hormone (PTH).
- This has the following effects:
- Effects of PTH on bone:
- Inhibits osteoblasts.
- Stimulates osteoclasts.
- Bone is broken down, releasing calcium ions into bloodstream.
- Effects of PTH on kidneys:
- PTH stimulates kidney tubule cells to recover waste calcium from the urine.
- PTH stimulates kidney tubule cells to release calcitriol.
- Effects of calcitriol on intestine:
- Stimulates intestines to absorb calcium from digesting food.
- Effects of PTH on bone:
- Blood calcium levels increase.
- Calcitonin release: high concentrations of calcium stimulate parafollicular cells in the thyroid to release calcitonin.
- Effects of calcitonin on bone:
-
- Stimulates osteoblasts.
- Inhibits osteoclasts.
- Calcium is removed from blood and used to build bone.
References
American Thyroid Association. (2019). Radioactive iodine. https://www.thyroid.org/radioactive-iodine/ ↵
DrugBank (2026). Levothyroxine. Levothyroxine: Uses, Interactions, Mechanism of Action | DrugBank
Eghtedari, B. & Correa, R. (2023). Levothyroxine. National Library of Medicine. StatPearls [Internet]. Levothyroxine – StatPearls – NCBI Bookshelf
McLaughlin, M. Awosika, A. & Jialal, I (2023). Calcitonin. National Library of Medicine. Calcitonin – StatPearls – NCBI Bookshelf
Vallerand, A. & Sanoski, C. (2024). Davis’s Canadian drug guide for nurses (19th ed.). F.A. Davis Company: Canada
Media Attributions
- “1811 The Thyroid Gland.jpg” by OpenStax College is licensed under CC BY 3.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/17-4-the-thyroid-gland ↵
- “1813 A Classic Negative Feedback Loop.jpg” by OpenStax College is licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/17-4-the-thyroid-gland ↵
- “Goitre.jpg” by Almazi is licensed under CC0 ↵
- American Thyroid Association. (2019). Radioactive iodine. https://www.thyroid.org/radioactive-iodine/ ↵
- “1814 The Parathyroid Glands.jpg” by OpenStax College is licensed under CC BY 3.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/17-5-the-parathyroid-glands ↵
- “1817 The Role of Parathyroid Hormone in Maintaining Blood Calcium Homeostasis.jpg” by OpenStax is licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/17-5-the-parathyroid-glands ↵
- “Levothyroxine 25mcg Tablets.jpg” by User:Ash is licensed under CC0 ↵
- “Nasal Spray” by NIAID is licensed under CC BY 2.0 ↵
- "1811 The Thyroid Gland.jpg" by OpenStax College is licensed under CC BY 3.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/17-4-the-thyroid-gland ↵
- "1813 A Classic Negative Feedback Loop.jpg" by OpenStax College is licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/17-4-the-thyroid-gland ↵
- American Thyroid Association. (2019). Radioactive iodine. https://www.thyroid.org/radioactive-iodine/ ↵
- "1814 The Parathyroid Glands.jpg" by OpenStax College is licensed under CC BY 3.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/17-5-the-parathyroid-glands ↵
- "1817 The Role of Parathyroid Hormone in Maintaining Blood Calcium Homeostasis.jpg" by OpenStax is licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/17-5-the-parathyroid-glands ↵

