12.6 Cephalosporins
Indications for Use
Cephalosporins are used to treat skin and skin-structure infections, bone infections, genitourinary infections, otitis media, and community-acquired respiratory tract infections. There are five generations of cephalosporins with many medications in each generation. They are widely used due to their broad range of coverage. In general, generation 1st and 2nd are effective against gram-positive cocci. The newer generations, 3rd-5th, have improved gram-negative coverage and CNS penetration (Bui, Patel & Preuss, 2024). More detail on specific coverage is below.
Mechanism of Action
Cephalosporins are typically bactericidal and are similar to penicillin in their action within the cell wall. They are beta-lactam antibiotics and are classified into five generations which is based on their antimicrobial properties. Higher generations generally have expanded spectra against aerobic gram-negative bacilli.
First generation drugs, such as cefazolin and cephalexin, are mainly effective against gram-positive organisms. Cefazolin is the cephalosporin of choice for surgical prophylaxis. They are also used for uncomplicated skin and soft tissue infections, such as cellulitis.
Second generation cephalosporins include cefuroxime. Second generation meds are less active against gram-positive cocci than first-generation cephalosporins but have improved activity against gram-negative bacilli. They are often prescribed to treat respiratory infections such as bronchiolitis or pneumonia.
Third generation includes ceftriaxone. They have extended gram-negative bacteria coverage, often used to treat gram-negative infections resistant to the first- and second-generation or other β-lactam antimicrobials. They can penetrate the blood brain barrier and are used of meningitis. Fourth-generation cephalosporin includes cefepime and is a broad-spectrum antimicrobial that can penetrate the cerebral spinal fluid (Bui, Patel & Preuss, 2024). The 5th-generation cephalosporins are active against methicillin-resistant Staphylococcus aureus (MRSA) or other complicated infections (Werth, 2018). 5th generation medications include ceftolozane.
Nursing Considerations
Lifespan:
- Pediatrics: most cephalosporins are considered safe for use with children.
- Older adult: some dose adjustments are required based on renal dysfunction in older adults. Older adults with CNS disorders are at risk for neurotoxicity.
- Pregnancy: Cephalosporins can typically be given during pregnancy, with monitoring.
Caution if consuming alcohol with a cephalosporin, in particular cefotetan and cefoperazone. There is a risk of disulfiram-like reactions including severe headache, flushing, nausea, vomiting, etc (Ren et al, 2014).
May interfere with coagulability and increase a client’s risk of bleeding.
Adverse/side effects:
Clients who are allergic to pencillin may also be allergic to cephalosporins. The most common side effects from cephalosporins are nausea, vomiting, lack of appetite, and abdominal pain.
Depending of the generation of cephalosporin, other adverse effects include:
- Vitamin K deficiency: some cephalosporins may inhibit vitamin K, leading to a decrease synthesis of coagulation factors.
- Hypersensitivity reactions: more common in first and second generation drugs, monitor for rash, hives and swelling.
- Disulfiram reaction: monitor for headache, flushing, nausea and vomiting.
- Drug induced hemolytic anemia
Bui, Patel & Preuss, 2024: Ren et al, 2014
Client Teaching
- Ensure to take the med as prescribed and to take the entire prescription even if they are feeling better.
- Avoid alcohol while on a cephalosporin: risk of a disulfiram reaction, which can occur when alcohol is ingested while taking the medication.
- Monitor for a rash and signs of superinfection (such as black, furry overgrowth on tongue; vaginal itching or discharge; loose or foul-smelling stool) and report to the prescribing provider.
- Taking a cephalosporin while breastfeeding is discouraged. It does enter breastmilk and may alter bowel flora of the infant (Vallerand & Sanoski, 2024).
Cephalosporin Medication Card
Now let’s take a closer look at the cephalosporin medication card (Daily Med, 2019). Because information about medication is constantly changing, nurses should always consult evidence-based resources to review current recommendations before administering specific medication.
Medication Card: Cephalosporins
Prototypes: 1st generation: cephalexin and Cefazolin; 2nd generation: cefprozil; 3rd generation: ceftriaxone; 4th generation: cefepime; 5th generation: ceftolozane
Mechanism of Action: Similar to penicillin. Bactericidal. Effective against streptococcus, staphylococcus organisms
Indications: UTIs, respiratory tract infections (pneumonia), ear infections, STIs. Prophylaxis pre→post surgery
Administration:
- Onset, peak and duration of action varies
- PO: Administer without regard to food; if GI distress, give with food. Well absorbed orally.
- IV: Reconstitute drug with sterile water or normal saline; shake well until dissolved. Inject into large vein or free-flowing IV solution over 3-5 minutes
- Geriatrics: may need dose adjustment d/t age-related ↓ in renal function
- OB, Lactating: ½ life ↓ & blood levels lower during pregnancy
Side Effects:
- CNS: Seizures, headaches
- GI: N/V, diarrhea (Diarrhea can start 4-5 days in)
- Derm: Stevens-Johnson syndrome, rashes
- Local: Pain @ IV site, Phlebitis @ IV site
SAFETY: If an allergic reaction occurs, antibiotic should be discontinued and appropriate therapy instituted. Serious anaphylactic reactions require emergency treatment with epinephrine and airway management.
Contraindications
- caution if penicillin allergy
- Lactam drug hypersensitivity: Pts allergic to penicillin ↑likely to be allergic to cephalosporins
- Hx of GI disease
Like penicillin:
- Other antibiotics = additive, inhibitory effects
- NSAIDs
- Oral birth control
- K+ supplements
Drug interaction with aminoglycosides or oral anti-coagulant drugs (eg warfarin)
Nursing Considerations
- Concurrent use of Loop diuretics and Aminoglycosides may ↑ risk of nephrotoxicity
- Alcohol should not be consumed until 72 hrs after stopping med.
- Monitor skin (rash, peeling skin), bowel (diarrhea, loose or bloody stools), hearing loss, breathing issues, seizures. Report any of these changes.
- Monitor for systemic signs of infections: elevated WBC count, fever, culture results.
Antimicrobial Med Cards
To support your learning, editable and printable drug cards for all the antimicrobials are available. Chapter 12 Antimicrobials Medication Cards. These drug cards are intended to support your learning and are not intended to replace accessing current drug guides prior to drug administration in practice.
Clinical Reasoning and Decision-Making Activity
Using the above information, consider the following clinical scenario question:
Mrs. Jenkins is an 89-year-old client admitted to the medical-surgical floor for treatment of a skin infection. The admitting provider prescribes Cefazolin 1 gram every 8 hours IV.
Mrs. Jenkins’ admission laboratory tests include renal laboratory studies reflecting:
- Creatinine: 120 μmol/L (Normal range: 50-110 μmol/L[7]
- Blood urea nitrogen (BUN): 10.5 mmol/L (Normal: 2.9-8.2 mmol/L)
- Glomerular Filtration Rate: 55 ml/min (Normal: 90-120 ml/min)[8]
On Day 3 Mrs. Jenkins has renal laboratory studies performed again. The results are:
- Creatinine: 150 μmol/L
- Blood urea nitrogen (BUN): 16.8 mmol/L
- Glomerular Filtration Rate: 20 ml/min
Are Day 3 findings expected or not? What course of action should the nurse take?
Note: Answers to the Clinical Reasoning Activities and Critical Thinking questions can be found in the Chapter 12: Antimicrobial Medications answer key – Fundamentals of Nursing Pharmacology – 2nd Canadian Edition section at the end of the book.
Image Description
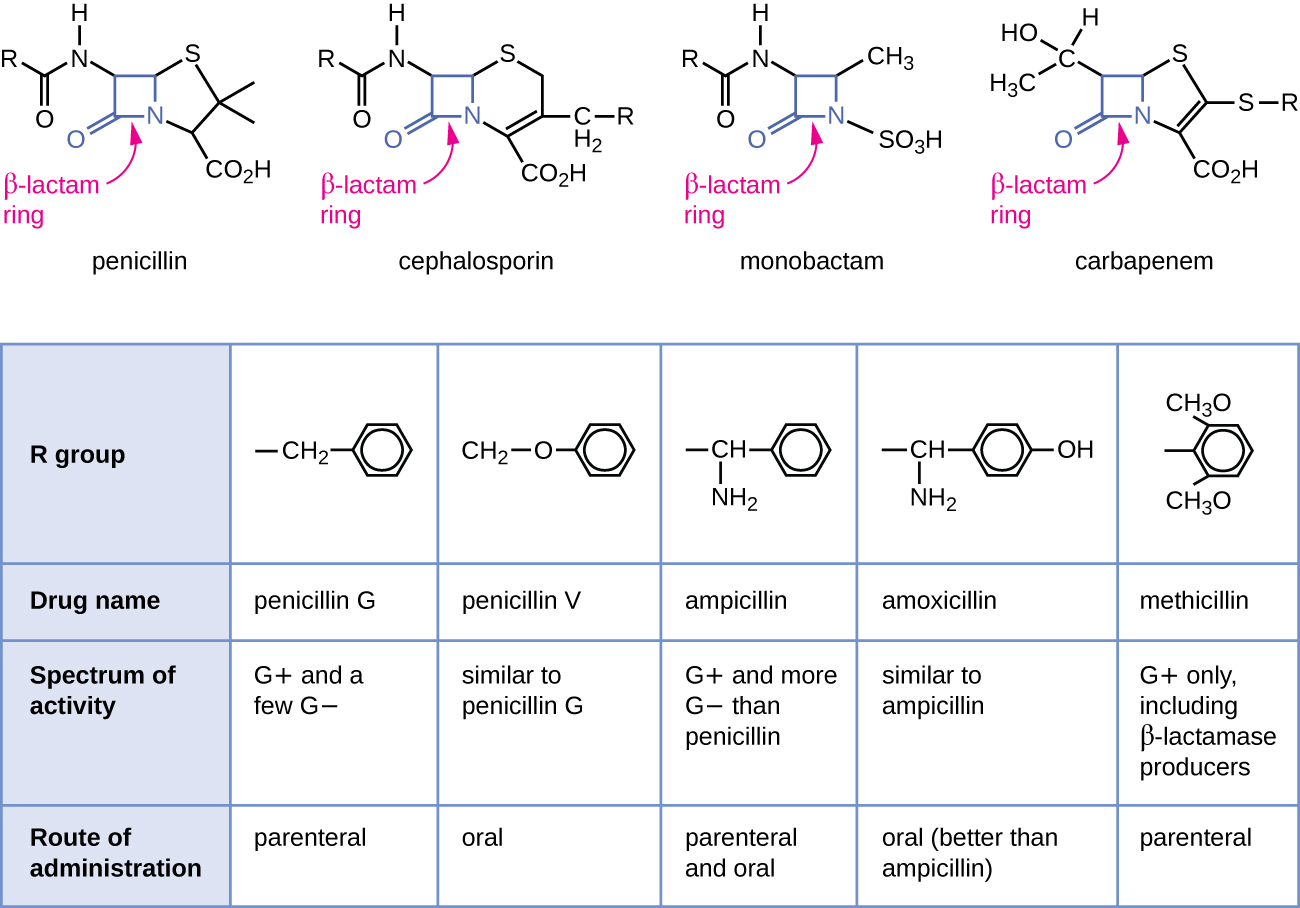
Figure 3.7 Comparison of beta-lactam ring structure across different classes of medications, spectrum of activity and routes of administration: Diagrams showing the chemical structures of various medication classes. These medications are:
- Penicillin.
- Cephalosporin.
- Monobactam.
- Carbapenem.
Each of these medications has a becta-lactam ring at the centre.
| Drug name | penicillin G | penicillin V | ampicillin | amoxicillin | methicillin |
|---|---|---|---|---|---|
| R group | CH2 | CH2 bonded to O | CH bonded to NH2 | CH bonded to NH2 on one side of the molecule, and OH bonded to the other side | CH3O bonded to one side of the molecule, and CH3O bonded to the other side |
| Spectrum of activity | G+ and a few G− | similar to penicillin G | G+ and more G− than penicillin | similar to ampicillin | G+ only, including β-lactamase producers |
| Route of administration | parenteral | oral | parenteral and oral | oral (better than ampicillin) | parenteral |
References
“OSC Microbio 14 02 BetaLactam.jpg” by CNX Openstax is licensed under CC BY 4.0 Access for free at https://openstax.org/books/microbiology/pages/14-3-mechanisms-of-antibacterial-drugs ↵
Bui, T., Patel, P. & Preuss, C. (2024). Cephalosporins. National Library of Medicine. StatPearls. Cephalosporins – StatPearls – NCBI Bookshelf
Ren, S., Cao, Y., Zhang, X., Jiao, S., Qian, S., & Liu, P. (2014). Cephalosporin induced disulfiram-like reaction: a retrospective review of 78 cases. International Surgery, 99(2), 142–146. https://www.internationalsurgery.org/doi/full/10.9738/INTSURG-D-13-00086.1 ↵
UpToDate (2021). <em>Cefazolin</em>. <a href=”https://www.uptodate.com/contents/search”>https://www.uptodate.com/contents/search</a> ↵
U.S. National Library of Medicine, Medline Plus. (2020, February 13). Basic metabolic panel. https://medlineplus.gov/ency/article/003462.htm ↵
U.S. National Library of Medicine, Medline Plus. (2020, February 13). Glomerular filtration rate. https://medlineplus.gov/ency/article/007305.htm ↵
Vallerand, A. & Sanoski, C. (2024). Davis’s Canadian drug guide for nurses (19th ed.). F.A. Davis Company: Canada
Werth, B.J. (2018, August). Cephalosporins. Merck Manual Professional Version. https://www.merckmanuals.com/professional/infectious-diseases/bacteria-and-antibacterial-drugs/cephalosporins ↵

