4.13 Beta-2 Agonists
Salbutamol is a bronchodilator that is a Beta-2 agonist. It is used for the treatment and prevention of bronchospasm. It is also called Albuterol, but that name is more commonly used in the US. For further information on this med class, go to chapter 8 Respiratory Medications.
Indications for Use
Salbutamol is commonly used to treat asthma and chronic obstructive pulmonary disease (COPD) to relieve bronchospasm. It can be used via inhalation to prevent exercise induced bronchospasm or used orally for long term treatment of bronchospasm.

Figure 4.13a Ventolin HFA (Albuterol Sulfate) Asthma Inhaler used for treating asthma as a rescue inhaler
Mechanism of Action
Salbutamol selectively binds to beta-2 adrenergic receptors in airway smooth muscle. This binding increases the formation of intracellular cAMP via stimulation of adenylyl cyclase which then leads to relaxing airway smooth muscle, inhibits the release of bronchoconstricting mediators from mast cells, and increases mucociliary transport. It also has a minor effect on Beta-1 receptors at higher doses, contributing to cardiovascular side effects.
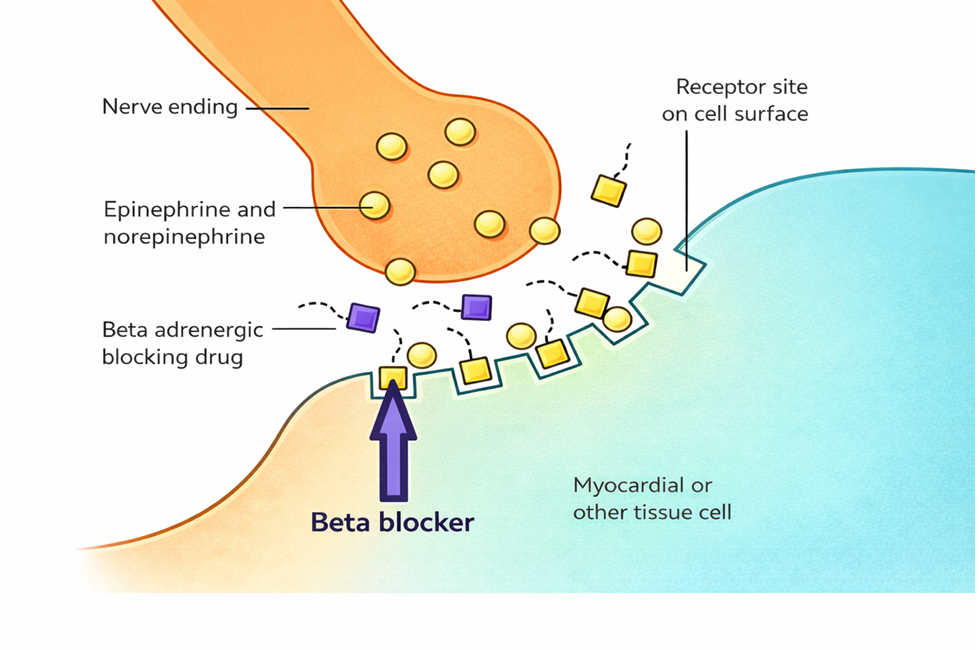
Figure 4.14b Beta adrenergic blocker mechanism of action (Sheila Odubote/ TRU Open Press).
Nursing Considerations
Administration: primarily inhalation and oral routes. Rarely given SQ, IM or IV.
- Inhalation: onset of action is 5-15 minutes, with a peak of 60-90 minutes. Duration of action is 3-6 hours. “Rescue” medication for acute bronchospasm. It has few side effects and no first pass metabolism.
- Oral: onset of action of 15-30 minutes with a peak of 2-3 hours. It has a long half-life, and easy to administer. Give with meals. Note that oral administration is less commonly prescribed.
Before and after administration:
- Monitor respiratory rate, oxygen saturation, and lungs sounds. If more than one inhalation is ordered, wait at least 1-2 minutes between inhalations. Use a spacer device to improve drug delivery, if appropriate.
Beta-2 agonists are safe for administration in pediatric and older adult populations, with appropriate dosing and scheduling.
Adverse/Side Effects
Adverse effects relate to stimulation of beta-2 receptors, which are located in skeletal vascular and bronchial smooth muscle, the liver, and on cell membranes
- paradoxical bronchospasm (with excess use). If wheezing develops, notify prescriber.
- May cause transient tachycardia/palpitations (direct stimulation of atrial beta-1 crossover effects) and tremors (beta-2 stimulation in skeletal muscle).
- Other CV: hypertension, chest pain, palpitations and arrhythmias.
- Risk of hyperglycemia. Monitor blood glucose more closely if diabetic.
- Hypokalemia (due to potassium entry into skeletal muscle)
May cause hypersensitivity reactions.
Client Teaching
- Follow instructions such as consistent dosing regimen. Do not double doses if a dose is missed.
- Use salbutamol first, then other inhalers.
- If symptoms not relieved by med or if they develop increased shortness of breath, contact prescriber.
- If using an inhaler:
- Prime the inhaler with 4 test sprays prior to administering the dose of medication or as per manufacturer’s instructions.
- Use a spacer to deliver medication
- May cause an unusual taste in the mouth, so rinsing mouth after use may reduce taste.
Salbutamol Medication Card
Now let’s take a closer look at the medication card on albuterol (UpToDate, 2021). Because information about medication is constantly changing, nurses should always consult evidence-based resources to review current recommendations before administering specific medication.
Downloadable file (.docx): Salbutamol Medication Card
Interactive Activity
References
uCentral from Unbound Medicine. https://www.unboundmedicine.com/ucentral ↵
UpToDate (2021). Albuterol. https://www.uptodate.com/contents/search
Vallerand, A. & Sanoski, C. (2024). Davis’s Canadian drug guide for nurses (19th ed.). F.A. Davis Company: Canada
Media Attributions
- Figure 4.13a Ventolin HFA (Albuterol Sulfate) Asthma Inhaler used for treating asthma as a rescue inhaler Creative Commons Attribution-Share Alike 4.0 International https://commons.wikimedia.org/wiki/File:Ventolin%C2%AE_HFA_(Albuterol_Sulfate)_Inhaler.jpg


