6.2 Conditions and Diseases of Pain and Mobility v2
Pain is a complex experience with biological, psychological and social/ environmental factors. It can range from mild and self-limiting, to debilitating effects that impact a client’s quality of life and functionality. Everyone experiences pain and it is listed as one of the top five reasons why people visit a primary care provider in Canada (Health Canada, 2019). In Canada, an estimated 7.6 million people across the lifespan live with chronic pain, and this number is expected to increase, partially due to our aging population (RNAO, 2024). Health Canada predicts that the number of Canadians living with chronic pain will rise by 17.5 per cent from 2019 to 2030 due to population growth (RNAO, 2024).
Nurses have a central role in pain assessment and management. Assessing pain is a component of every assessment and often has an impact on unrelated health conditions. As such, nurses need to have a good understanding of the types of pain, and common conditions that can exhibit unique pain experiences. In this unit, we will provide a brief overview of several conditions that cause pain or inflammation that require the use of analgesics or musculoskeletal medication. Common disorders are briefly reviewed below.
Types of Pain
A number of terms are often used to describe the pain a client is experiencing. There are three primary types of pain, based on how long the pain lasts and its frequency (National Institute of Neurological Disorders and Stroke, n.d.). These are acute pain, chronic pain, and episodic pain (periodic, occurs in intervals). Pain can also be categorized based on the source of pain, and include nociceptive, neuropathic and nociplastic. The more common terms will be explained below.
Acute pain
Acute pain usually comes on suddenly and is caused by something specific. It is sharp in quality. Acute pain usually does not last longer than four weeks (Province of BC, 2022). It goes away when there is no longer an underlying cause for the pain. Causes of acute pain are typically due to injuries, illnesses, surgeries or other medical procedures, and resolve with tissue healing. For example, from dental work, burns or cuts, infections, or labor and childbirth. After acute pain goes away, a person can go on with life as usual (Cleveland Clinic, 2017).
Subacute pain
Subacute pain is defined as pain in the transition between acute and chronic. It does not resolve or diminish as expected within a 4–12-week period after the initial onset. During this time, health care practitioners should be reviewing the treatment strategies and take steps to minimize the transition to chronic pain (Province of BC, 2022).
Chronic pain
Chronic pain is pain that is ongoing and usually lasts longer than three months. This type of pain can continue even after the injury or illness that caused it has healed or gone away. Pain signals remain active in the nervous system for weeks, months, or years. Some people suffer chronic pain even when there is no past injury or apparent body damage. Chronic pain is linked to conditions including:
- Headache
- Arthritis
- Cancer
- Nerve pain
- Back pain
- Fibromyalgia pain
- Phantom pain
People who have chronic pain can experience physical effects that are stressful on the body. These include tense muscles, limited ability to move around, a lack of energy, and appetite changes. Emotional effects of chronic pain include depression, anger, anxiety, and fear of reinjury. Such a fear might limit a person’s ability to return to their regular work or leisure activities (Cleveland Clinic, 2017).
Chronic pain is a significant health issue in Canada. It is estimated that one in five (across their lifespan) or 7.6 million Canadians live with chronic pain (Province of BC, 2022). Managing chronic pain requires an individualized treatment plan that applies a trauma informed approach with the goal of improving functionality and addressing pain, disability and suffering (Province of BC, 2022).
Neuropathic Pain:
Neuropathic pain is caused by nerve damage from a lesion, injury or disease. This type of pain are often described as burning, tingling, shooting, or like electric shocks. Examples of conditions that cause neuropathic pain are diabetic neuropathy, shingles, and sciatica (RNAO, 2024).
Nociceptive Pain:
Nociceptive pain describes pain that is caused by tissue damage and/or inflammation to non-neural tissue and is due to activation of nociceptors. The sensation can be sharp, pricking, dull, or aching, depending on what caused the damage or inflammation. Examples of nociceptive pain are pain from a physical injuries such as a paper cut, an infection, a broken bone, or osteoarthritis. It can also be from chemical agents such as a burn (National Institute of Neurological Disorders and Stroke, n.d.).
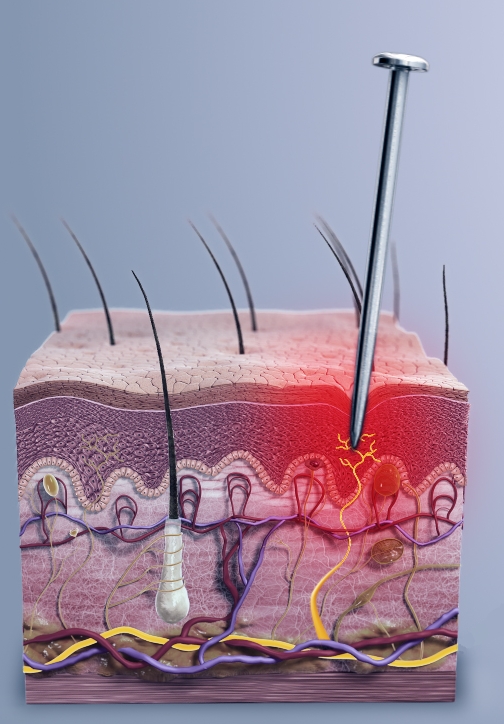
Figure 6.2a nociceptive pain
File:Nociceptive pain 2.jpg . This file is licensed under the Creative Commons Attribution-Share Alike 4.0 International license. Original file (504 × 724 pixels, file size: 234 KB, MIME type: image/jpeg)
Nociceptive pain is caused by the activation of pain receptors, called nociceptors, in response to actual or threatened tissue damage from events like cuts, burns, or sprains. Nociceptors are stimulated when the nail pierces the skin and tissue, sending pain signals to the brain.
Other Conditions of Pain and Mobility
Fibromyalgia is a condition that causes pain all over the body (widespread pain), sleep problems, fatigue, and often emotional and mental distress. People with fibromyalgia may be more sensitive to pain than people without fibromyalgia. This is called abnormal pain perception processing. Fibromyalgia affects about 4 million US adults, about 2% of the adult population. The cause of fibromyalgia is not known, but it can be effectively treated and managed (Centers for Disease Control and Prevention, 2017).
The most common symptoms of fibromyalgia are the following:
- Pain and stiffness all over the body
- Fatigue and tiredness
- Depression and anxiety
- Sleep problems
- Problems with thinking, memory, and concentration
- Headaches, including migraines
Other symptoms may include:
- Tingling or numbness in hands and feet
- Pain in the face or jaw, including disorders of the jaw known as temporomandibular joint syndrome (TMJ)
- Digestive problems, such as abdominal pain, bloating, constipation, and even irritable bowel syndrome (IBS)
Known risk factors include:
- Age. Fibromyalgia can affect people of all ages, including children. However, most people are diagnosed during middle age
- Lupus or Rheumatoid Arthritis. Clients diagnosed with lupus or rheumatoid arthritis (RA) are more likely to develop fibromyalgia
Other factors that have been weakly associated with the onset of fibromyalgia include:
- Sex. Women are twice as likely to have fibromyalgia as men
- Stressful or traumatic events, such as car accidents or post-traumatic stress disorder (PTSD)
- Repetitive injuries. Injury from repetitive stress on a joint, such as frequent knee bending
- Illness (such as viral infections)
- Family history
- Obesity
Doctors usually diagnose fibromyalgia using the client’s history, physical examination, X-rays, and blood work (Centers for Disease Control and Prevention, 2017).
Gout
Gout is a common form of inflammatory arthritis that is very painful. It usually affects one joint at a time (often the big toe joint). There are times when symptoms get worse, known as flares, and times when there are no symptoms, known as remission. Repeated bouts of gout can lead to gouty arthritis, a worsening form of arthritis.
There is no cure for gout, but you can effectively treat and manage the condition with medication and self-management strategies.
Gout flares start suddenly and can last days or weeks. These flares are followed by long periods of remission (weeks, months, or years) without symptoms before another flare begins. Along with the big toe, joints commonly affected are the lesser toe joints, the ankle, and the knee (Centers for Disease Control and Prevention, 2019, January 28).
Symptoms in the affected joint(s) may include:
- Pain, usually intense
- Swelling
- Redness
- Heat
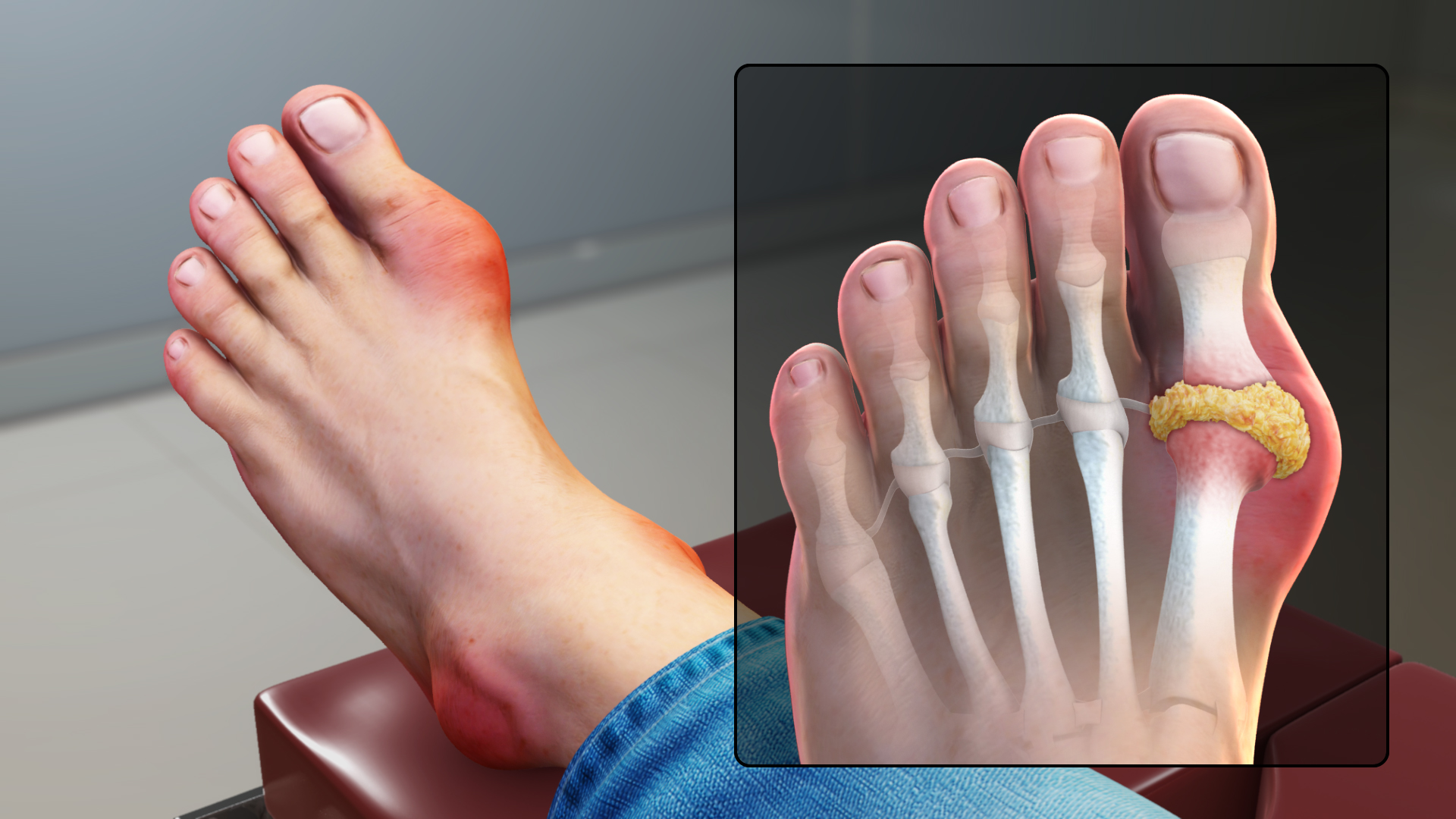
Gout is caused by a condition known as hyperuricemia, where there is too much uric acid in the body. The body makes uric acid when it breaks down purines, which are found in your body and the foods you eat. When there is too much uric acid in the body, uric acid crystals (monosodium urate) can build up in joints, fluids, and tissues within the body. Hyperuricemia does not always cause gout, and hyperuricemia without gout symptoms does not need to be treated. There is a higher incidence of gout in males.
Having certain health conditions can also increase your chances of developing hyperuricemia. These conditions include the following:
- Congestive heart failure
- Hypertension (high blood pressure)
- Insulin resistance
- Metabolic syndrome
- Diabetes
- Poor kidney function
- Obesity
Additional diet or medication factors may increase your chances of developing hyperuricemia:
- Using certain medications, such as diuretics (water pills)
- Drinking alcohol. The risk of gout is greater as alcohol intake increases
- Eating or drinking food and drinks high in fructose (a type of sugar)
- Having a diet high in purines, which the body breaks down into uric acid. Purine-rich foods include red meat, organ meat, and some kinds of seafood, such as anchovies, sardines, mussels, scallops, trout, and tuna.
A medical doctor diagnoses gout by assessing your symptoms and the results of your physical examination, X-rays, and lab tests. Gout can only be diagnosed during a flare when a joint is hot, swollen, and painful and when a lab test finds uric acid crystals in the affected joint (Centers for Disease Control and Prevention, 2019, January 28).
Muscle spasm
Muscle spasms are involuntary contractions of a muscle or group of muscles (Adams et al, 2019). Spasms of skeletal muscles are most common and are often due to overuse leading to muscle fatigue, but can also be attributed to dehydration, and electrolyte abnormalities. Some medications can lead to muscle spasms such as corticosteroids and anti-lipid medication such as statins. Diseases such as multiple sclerosis can also lead to chronic muscle spasms.
The spasm often occurs abruptly, is painful, and is usually short-lived (Wedro, 2019). Other symptoms may include inflammation, edema, loss of coordination or decreased mobility (Adams et al, 2019). If persistent or moderate to severe discomfort, non-pharmacological and pharmacological interventions can be tried. Non-pharmacological interventions may include gentle stretching of the muscle, application of heat or cold, rest, massage or acupuncture. Medications can include centrally acting skeletal muscle relaxants such as baclofen or cyclobenzaprine.
Multiple Sclerosis
Multiple sclerosis (MS) involves an immune-mediated disease process in which an abnormal response of the body’s immune system is directed against the central nervous system (CNS). The CNS is made up of the brain, spinal cord, and optic nerves.
Within the CNS, the immune system causes inflammation that damages myelin (the fatty substance that surrounds and insulates the nerve fibers), as well as the nerve fibers themselves and the specialized cells that make myelin. When myelin or nerve fibers are damaged or destroyed in MS, messages within the CNS are altered or stopped completely. Damage to areas of the CNS may produce a variety of neurological symptoms that will vary among people with MS in type and severity. The damaged areas develop scar tissue that gives the disease its name – multiple areas of scarring or multiple sclerosis. The cause of MS is not known, but it is believed to involve genetic susceptibility, abnormalities in the immune system, and environmental factors that combine to make MS symptoms variable and unpredictable. No two people have exactly the same symptoms, and each person’s symptoms can change or fluctuate over time. One person might experience only one or two of the possible symptoms, while another person might experience several symptoms of the disease.
Symptoms include:
- Fatigue
- Numbness or tingling
- Weakness
- Dizziness or vertigo
- Walking difficulties
- Muscle spasticity
- Blurred vision
At this time, there are no symptoms, physical findings, or laboratory tests that can, by themselves, determine if a person has MS. Several strategies are used to determine if a person meets the long-established criteria for a diagnosis of MS and to rule out other possible causes of whatever symptoms they are experiencing. These strategies include a careful medical history, a neurologic exam, and various tests including magnetic resonance imaging (MRI), spinal fluid analysis, and blood tests (National Multiple Sclerosis Society, 2018).
Myasthenia Gravis
Myasthenia Gravis (MG) is an autoimmune disease that occurs when the immune system attacks the body’s own tissues. In MG, the attack interrupts the connection between nerve and muscle called the neuromuscular junction. Myasthenia gravis is characterized by autoantibodies against the acetylcholine receptor or against a receptor-associated protein called muscle-specific tyrosine kinase. You can read more details about acetylcholine receptors in the “Autonomic Nervous System” chapter.
MG causes weakness in muscles that control the eyes, face, neck, and limbs. Symptoms include partial paralysis of eye movements, double vision, and droopy eyelids, as well as weakness and fatigue in the neck and jaws and problems, chewing, swallowing, and holding up the head. MG is treatable with drugs that suppress the immune system or boost the signals between nerve and muscle (Muscular Dystrophy Association, n.d.). The group of drugs used to control MG is called acetylcholinesterase (ACh) inhibitors. They inhibit the action of the enzyme acetylcholinesterase so that more acetylcholine (ACh) is available to activate cholinergic receptors and promote muscle contraction. ACh inhibitors are classified as parasympathomimetics. Pyridostigmine is an example of an ACh inhibitor.
Overdosing with ACh inhibitors can cause a complication called cholinergic crisis, which is an acute exacerbation of symptoms. A cholinergic crisis usually occurs 30-60 minutes after taking cholinergic medication with severe muscle weakness that can lead to respiratory paralysis and death (McCuistion, 2018).
References
Cleveland Clinic. (2017, January 26). Acute v. chronic pain. https://my.clevelandclinic.org/health/articles/12051-acute-vs-chronic-pain ↵
Centers for Disease Control and Prevention. (2017, October 11). Arthritis, Fibromyalgia. https://www.cdc.gov/arthritis/basics/fibromyalgia.htm ↵
Centers for Disease Control and Prevention. (2019, January 28). Arthritis, Gout. https://www.cdc.gov/arthritis/basics/gout.html ↵
Health Canada (2019). Canadian Pain Task Force Report. Canadian Pain Task Force Report: June 2019 – Canada.ca
National Multiple Sclerosis Society. (2018, March 8). What is MS? [Video]. YouTube. All Rights Reserved. https://youtu.be/geQP_zYS-6s ↵
Muscular Dystrophy Association. (n.d.). Myasthenia gravis. https://www.mda.org/disease/myasthenia-gravis ↵
McCuistion, L., Vuljoin-DiMaggio, K., Winton, M, & Yeager, J. (2018). Pharmacology: A patient-centered nursing process approach. pp. 268-270, 324, 332. Elsevier.
National Institute of Neurological Disorders and Stroke (n.d.). Pain. Pain | National Institute of Neurological Disorders and Stroke
Province of BC (2022, Feb 22). Managing patients with pain in primary care – part 1. BC Guidelines.ca https://www2.gov.bc.ca/gov/content/health/practitioner-professional-resources/bc-guidelines/managing-patients-with-pain-in-primary-care-part-1
Registered Nurses Association of Ontario (RNAO). (2024). Pain, Prevention, Assessment and Management (4th ed.) Toronto (ON): RNAO.
Wedro, B. (2019, July 18). Muscle spasms. https://www.medicinenet.com/muscle_spasms/article.htm. ↵
Images
Scientific Animations (2019). Gout: signs or symptoms. Retrieved from Wikipedia Commons File: Gout Signs and Symptoms.jpg http://www.scientificanimations.com/wiki-images/
Pain that usually starts suddenly and has a known cause, like an injury or surgery. It normally gets better as your body heals and lasts less than three months.
Pain that lasts 6 months or more and can be caused by a disease or condition, injury, medical treatment, inflammation, or an unknown reason.
Occurs when the body's immune system attacks the central nervous system.
A sense of spinning dizziness. It is a symptom of a range of conditions. It can happen when there is a problem with the inner ear, brain, or sensory nerve pathway.
Condition in which certain muscles are continuously contracted. This contraction causes stiffness or tightness of the muscles and can interfere with normal movement, speech, and gait. Spasticity is usually caused by damage to the portion of the brain or spinal cord that controls voluntary movement.

