10.2 Conditions and Diseases Related to the Endocrine System V2
Andrea:Amanda Egert; Kimberly Lee; and Manu Gill not sure if we keep these authors, or add my name for the revision?
Jessica/Mar 16: I have removed the names of the previous authors from version 1
As you have just learned, the endocrine system regulates vital hormonal and enzymatic functions. Individuals with metabolic regulation disorders have trouble regulating one or more of these functions. Disorders can be related to hyposecretion, hypersecretion or hyporesponsiveness. Sometimes the cause is primary, such when the gland releases an inadequate amount of hormone or it can be secondary, when the tropic hormone fails to cause the target gland to secrete adequate amounts of the hormone. Hyporesponsiveness is related to a deficiency in cellular receptors, leading to hyposecretion (Copstead & Banisik, 2010). Cushing’s disease is an example of hypersecretion where the pituitary gland becomes hyperactive and oversecretes ACTH, which induces the adrenal cortex to produce too much cortisol. This chapter will focus on metabolic regulation related to adrenal gland disorders, diabetes and thyroid disorders (Karch, 2017).
Disorders Involving the Adrenal Glands
Several disorders are caused by the dysregulation of the hormones produced by the adrenal glands. Dysregulation can occur with any of the hormones. Some conditions include:
- Acromegaly: this is a condition of hypersecretion of the growth hormone. This leads to an increase in size of bones, cartilage, body organs and other tissues. It can occur in both children and adults, and is rare. It can also lead to many other health issues such as arthritis, type 2 diabetes, hypertension and heart disease (National Institute of Diabetes and Digestive and Kidney Diseases (NIDDKD), 2020).
- Grave’s Disease: this is an autoimmune disorder that can cause hyperthyroidism. It is due to the immune system attacking the thyroid gland, leading to many body functions speeding up. If left untreated, it can lead to osteoporosis, irregular heart rate, vision changes and menstrual irregularities (NIDDKD, 2020).
- Lack of aldosterone secretion or hypoaldosteronism, can be due to a few different disorders. It can be due to hyposecretion of aldosterone (Addison’s Disease), decreased stimulation of the adrenal cortex or aldosterone resistance. Sometimes the causes are medication related, such as suddenly stopping steroid therapy or due to diseases of the renal tubules. Addison’s disease can be caused by an autoimmune disorder, and presents with symptoms such as hypoglycemia, hyponatremia, fatigue, muscle weakness and weight loss. In any case, finding the cause is important, and treating with a mineralocorticoid and low dose corticosteroid may be prescribed (Adams et al, 2018).
- Hypersecretion of glucocorticoids: Cushing’s disease is a disorder that most often is due to long-term, high-dose use of glucocorticoids. Rarely it is due to adrenal tumours or other endogenous causes (NIDDKD, 2020). It is characterized by high blood glucose levels, the development of a moon-shaped face, a buffalo hump on the back of the neck, rapid weight gain, and hair loss (Lui et al, 2015; Neiman et al, 2015)
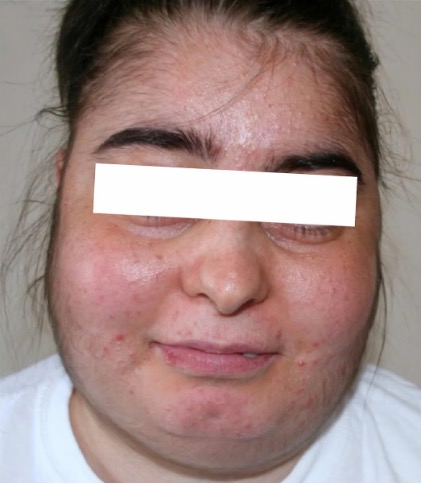
Moon face in Cushing’s syndrome By Ozlem Celik, Mutlu Niyazoglu, Hikmet Soylu and Pinar Kadioglu. License: CC BY 2.5 måneansigt – Lex
Disorders of the Endocrine System: Diabetes Mellitus
Dysfunction of insulin production and secretion, as well as the target cells’ responsiveness to insulin, can lead to a condition called diabetes mellitus, a common disease that affects the ability of the body to produce and/or utilize insulin. There are two main forms of diabetes mellitus.
Type 1 Diabetes is an autoimmune disease affecting the beta cells of the pancreas. The beta cells of people with type 1 diabetes do not produce insulin; thus, synthetic insulin must be administered by injection or infusion. Presenting symptoms include polyuria, polydipsia, and polyphagia. Clients may also have unexplained weight loss and blurred vision. If left untreated the client can go into ketoacidosis, a life-threatening condition.
Type 2 Diabetes accounts for approximately 95 percent of all cases. It is acquired, with contributing factors of family history, over the age of 40, overweight, and lifestyle factors such as poor diet and inactivity greatly increase a person’s risk (Diabetes Care Community, 2023). In type 2 diabetes, the body’s cells become resistant to the effects of insulin. In response, the pancreas increases its insulin secretion, but over time, decompensation occurs as the impaired beta cells are unable to produce sufficient insulin to overcome insulin resistance. In many cases, type 2 diabetes can be reversed by moderate weight loss, regular physical activity, and consumption of a healthy diet. However, if blood glucose levels cannot be controlled, oral diabetic medication is prescribed.
Type 2 diabetes is a progressive disease, especially if blood sugars are not kept within target range. The client often begins with one oral anti-diabetic medication, and may be prescribed additional meds depending on their blood sugars, other health issues and symptom management. As with type 1 diabetes, blood sugar control is essential to avoid hypoglycemia and hyperglycemia fluctuations. Over time, long term physiological changes can occur such as retinopathy, neuropathies, nephropathy leading to kidney failure and cardiovascular disease.
Diagnosis of Diabetes
Screening for type 2 diabetes should be done every 3 years for individuals over 40 years of age or anyone considered high risk of developing diabetes. If a client has numerous risk factors, screening may be done q 6-12 months or by the recommendation of their health care provider.
Screening includes fasting plasma glucose and/or glycated hemoglobin (A1C).
High risk factors include: family history of diabetes, history of pre-diabetes or gestational diabetes, overweight, or a member of a high-risk group: African, Arab, Asian, Hispanic, Indigenous or South Asian descent, low socioeconomic status (Diabetes Canada Clinical Practice Guidelines Expert Committee, 2026).
| Fasting blood glucose levels (FBG) | Normal: less than 5.6 mmol/L
At risk: 5.6-6.0 mmol/L Pre-diabetes: 6.1 to 6.9 mmol/L Diabetes: greater than 7.0 mmol/L
|
Fasting at least 8 hours.
(Slight differences in values between some sources. Normal FBG 4.0-7.0 reported with Diabetes Canada) |
| Random blood glucose test
|
Diabetes: 11.1 mmol/L or higher. | No fasting or preparation involved. |
| Oral glucose tolerance test (OGTT)
|
Following ingesting 75 grams of glucose in a drink, after 2 hours:
Diabetes: BG level 11.1 mmol/L or higher Pre-diabetes: 7.8 – 11.0 mmol/L |
measures your body’s ability to use glucose.
Plasma glucose level drawn, followed by a 75 gram glucose load, then second blood glucose level. |
| Glycosylated hemoglobin, also called A1C | Normal: under 5.5%
At risk: 5.5-5.9% Pre-diabetes: 6-6.4% Diabetes: greater than 6.5%
|
Used to assess long-term blood glucose levels over 3 months. Good indicator of blood glucose control.
(Normal under 6.5% with Diabetes Canada) |
For more information on diabetes management in Canada, go to the Diabetes Canada website: About diabetes – Diabetes Canada this is an excellent resource for clients and health care professionals.
Disorders of the Thyroid Gland: Iodine Deficiency, Hypothyroidism, and Hyperthyroidism
Hyposecretion of the thyroid gland results in an inadequate amount of serum thyroid hormone to meet the physiological needs. Inflammation of the thyroid gland is a common cause of hypothyroidism, or low blood levels of thyroid hormones. Hypothyroidism is a disorder characterized by a low metabolic rate, weight gain, cold extremities, constipation, reduced libido, menstrual irregularities, and reduced mental activity, and requires long-term thyroid hormone replacement therapy, such as thyroxine.
In contrast, hyperthyroidism—an abnormally elevated blood level of thyroid hormones—is often caused by a pituitary or thyroid tumor. In Graves’ disease, the hyperthyroid state results from an autoimmune reaction in which antibodies overstimulate the follicle cells of the thyroid gland. Symptoms of hyperthyroidism include an increased metabolic rate, excessive body heat and sweating, diarrhea, weight loss, tremors, and increased heart rate. The person’s eyes may bulge (called exophthalmos) as antibodies produce inflammation in the soft tissues of the orbits. The person may also develop a goiter.
Treatment for Hyperthyroidism is thyroid surgery or with radioactive iodine (RAI) therapy. Patients are asked to follow radiation precautions after RAI treatment to limit radiation exposure to others, especially pregnant women and young children, such as sleeping in a separate bed and flushing the toilet 2-3 times after use. The RAI treatment may take up to several months to have its effect. The end result of thyroid surgery or RAI treatment is often hypothyroidism, which is treated by thyroid hormone replacement therapy (American Thyroid Association, 2019).
Other Metabolic Regulation Conditions and Disorders
This unit has provided a brief overview of common health issues related to the endocrine system. For a more detailed understanding of these conditions, refer to relevant resources. Due to the limited scope of this textbook, we will not be discussing other metabolic regulation disorders. If you are interested, consider reviewing resources on the following disorders: Hyper and hypoglycemia, gestational diabetes, diabetic insipidus, diabetic ketoacidosis, and parathyroid disorders.
Media Attributions
- Figure 10.3a Moon face in Cushing’s syndrome By Ozlem Celik, Mutlu Niyazoglu, Hikmet Soylu and Pinar Kadioglu. License: CC BY 2.5 måneansigt – Lex
References
- Adams, M., Urban, C., El-Hussein, M., Osuji, J. & King, S. (2018). Pharmacology for Nurses. A pathophysiological approach (2nd Canadian ed.). Pearson Canada Inc: Ontario
- American Thyroid Association. (2019). Radioactive iodine. https://www.thyroid.org/radioactive-iodine/ ↵
- Copstead, L. & Banisik, J. (2010). Pathophysiology (4th ed.). Missouri: Elsevier.
- Diabetes (2020). Diabetes: Blood Sugar Levels. https://www.healthlinkbc.ca/illnesses-conditions/diabetes/diabetes-blood-sugar-levels ↵
- Diabetes Canada Clinical Practice Guidelines Expert Committee (2026). Clinical Practice Guidelines. Diabetes Canada. Diabetes Canada | Clinical Practice Guidelines
- Diabetes Care Community (2023). Blood sugar levels in Canada. Blood Sugar Levels In Canada
- Karch, A. (2017). Focus On Nursing Pharmacology. Philadelphia: Wolters Kluwer.
- Liu, D., Ahmet, A., Ward, L., Krishnamoorthy, P., Mandelcorn, E., Leigh, R., Brown, J., Cohen, A., & Kim, H. (2013, August 15). A practical guide to the monitoring and management of the complications of systemic corticosteroid therapy. Allergy, Asthma & Clinical Immunology, 9(30). https://doi.org/10.1186/1710-1492-9-30 ↵
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDKD), (2020). Endocrine Diseases. Cushing’s Syndrome – NIDDK
- Nieman, L., Biller, B., Findling, J., Murad, M., Newell-Price, J., Savage, M, & Tabarin, A. (2015, August 1). Treatment of Cushing’s Sydnrome: an endocrine clinical practice guideline. The Journal of Clinical Endocrinology & Metabolism, 100(8). pp. 2807-2831. https://academic.oup.com/jcem/article/100/8/2807/2836065 ↵
- Open Stax, (2022). Anatomy and Physiology licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/1-introduction ↵
Abnormally low blood levels of thyroid hormones T3 and T4 in the bloodstream.
Abnormally elevated blood level of thyroid hormones T3 and T4, often caused by a pituitary tumor, thyroid tumor, or autoimmune reaction in which antibodies overstimulate the follicle cells of the thyroid gland

