10.1 Metabolic Regulation Concepts V2
Concepts Related to Metabolic Regulation
For the purposes of this concept discussion, the Concept of Metabolic Regulation is defined as the regulation of hormonal and enzymatic processes required to maintain homeostasis (Giddens, 2017, pg. 241). This unit will review the concepts related to hormone regulation. This will include hypothalamus-pituitary gland complex and a review of the hormones and function of two glands, the pituitary and adrenals. A review of the pancreas, particularly related to glucose regulation will be reviewed in the subsequent chapter, chapter 11, Endocrine System: glucose regulation and anti-diabetic medications.
You may never have thought of it this way, but when you send a text message to two friends to meet you at a restaurant at six, you’re sending digital signals that you hope will affect their behavior—even though they are some distance away. Similarly, certain cells send chemical signals to other cells in the body that influence their behavior. This long-distance intercellular communication, coordination, and control are critical for homeostasis, and it is the fundamental function of the endocrine system. Whereas the nervous system uses neurotransmitters to communicate, the endocrine system uses hormones for chemical signaling. These hormone signals are sent by the endocrine organs.
Hormones are transported primarily via the bloodstream throughout the body, where they bind to receptors on target cells, inducing a characteristic response. Some of the glands in the endocrine system include the pituitary, thyroid, parathyroid, adrenal, and pineal glands. Some of these glands have both endocrine and nonendocrine functions. For example, the pancreas contains cells that function in digestion, as well as cells that secrete the hormones insulin and glucagon, which regulate blood glucose levels (Open Stax, 2022).
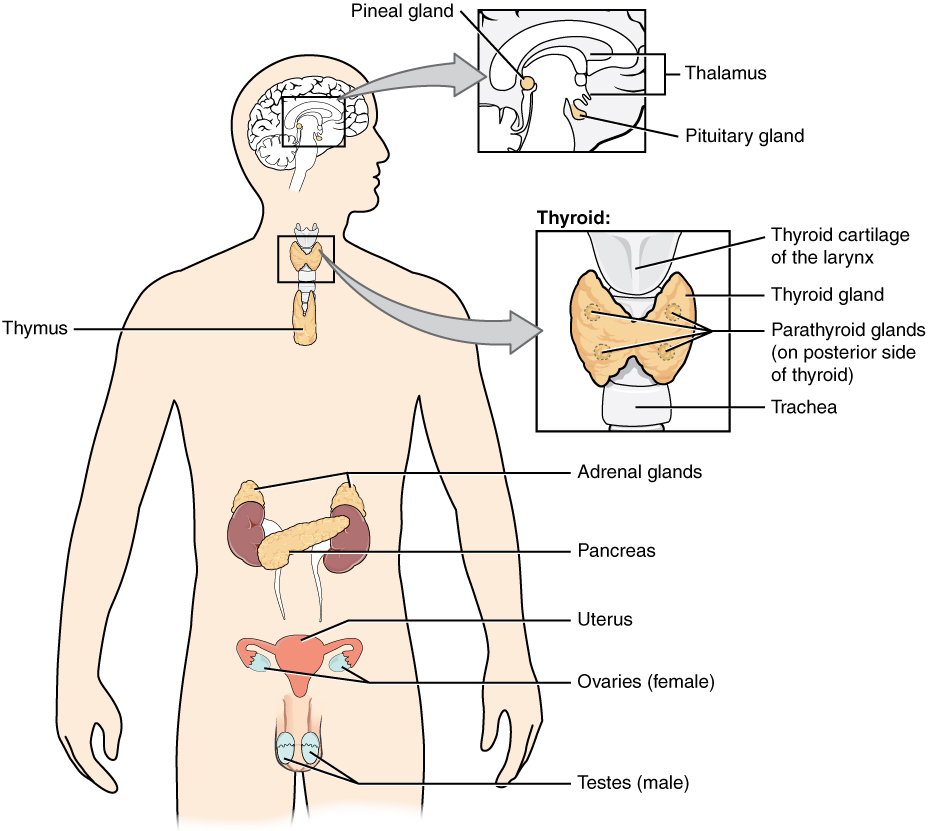
What is a hormone?
Hormones are molecules produced by various endocrine glands, which are then carried by the blood to their target cells. A hormone can have very specific target cells or affect numerous cell types throughout the body. Once the hormone binds with the receptor site on a cell, it triggers a cascade of reactions in the target cell resulting in modifying the cell’s function or activity.
This module will focus on medications that affect three major endocrine glands and their hormones: the adrenal glands, the pancreas, and the thyroid. See Table 10.2 for a list of hormones associated with each of these glands and their effects.
| Endocrine gland | Hormone | Primary Hormone Function |
| Adrenal (cortex) | Aldosterone | Helps control the body’s water and electrolyte regulation. Increases blood Na+ levels |
| Adrenal (cortex) | Cortisol | Helps control carbohydrate, protein and lipid metabolism; Increases blood sugar levels. Protects against stress. |
| Adrenal (medulla) | Epinephrine and Norepinephrine | Stimulates fight-or-flight response |
| Pancreas | Insulin | Helps control carbohydrate metabolism; reduces blood glucose levels |
| Pancreas | Glucagon | Helps control carbohydrate metabolism; Increases blood glucose levels |
| Thyroid | Thyroxine (T4), triiodothyronine (T3) | Controls metabolic processes in all cells; stimulates basal metabolic rate |
| Thyroid | Calcitonin | Helps control calcium metabolism; reduces blood Ca+ levels |
Regulation of Hormone Secretion
To prevent abnormal hormone levels and a potential disease state, hormone levels must be tightly controlled. Feedback loops govern the initiation and maintenance of hormone secretion in response to various stimuli.
The most common method of hormone regulation is the negative feedback loop. Negative feedback is characterized by the inhibition of further secretion of a hormone in response to adequate levels of that hormone. This allows blood levels of the hormone to be regulated within a narrow range. An example of a negative feedback loop is the release of glucocorticoid hormones from the adrenal glands, as directed by the hypothalamus and pituitary gland. As glucocorticoid concentrations in the blood rise, the hypothalamus and pituitary gland reduce their signaling to the adrenal glands to prevent additional glucocorticoid secretion (Open Stax, 2022).
See Figure 10.1b for an illustration of a negative feedback loop (Open Stax, 2022).
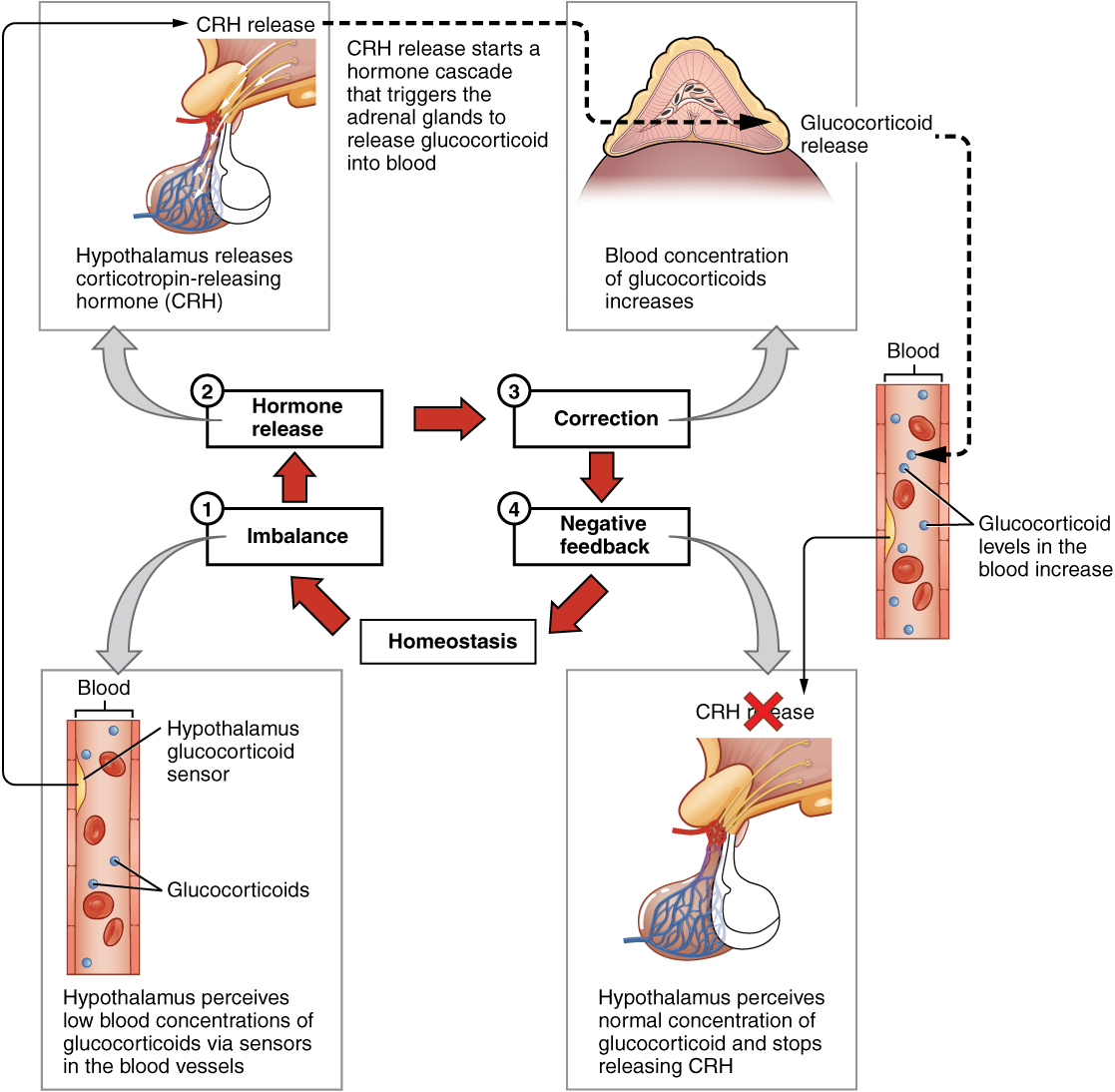
Endocrine Gland Stimuli
Endocrine glands can be stimulated by humoral stimuli, by stimulation of another hormone, or by neural stimuli. Humoral stimuli are changes in blood levels of non-hormone chemicals that cause the release or inhibition of a hormone to maintain homeostasis. For example, osmoreceptors in the hypothalamus detect changes in blood osmolarity (the concentration of solutes in the blood plasma). If blood osmolarity is too high, meaning that the blood is not dilute enough, osmoreceptors signal the hypothalamus to release ADH (antidiuretic hormone). ADH causes the kidneys to reabsorb more water and reduce the volume of urine produced. This reabsorption causes a reduction of the osmolarity of the blood by diluting the blood to the appropriate level. Another example of humoral stimuli is the regulation of blood glucose. High blood glucose levels cause the release of insulin from the pancreas, which increases glucose uptake by cells and liver storage of glucose as glycogen.
An endocrine gland may also secrete a hormone in response to the presence of another hormone produced by a different endocrine gland. For example, the thyroid gland secretes T4 into the bloodstream when triggered by thyroid-stimulating hormone (TSH) that is released from the anterior pituitary gland.
In addition to these chemical signals, hormones can also be released in response to neural stimuli. An example of neural stimuli is the activation of the fight-or-flight response by the sympathetic nervous system. When an individual perceives danger, sympathetic neurons signal the adrenal glands to secrete norepinephrine and epinephrine. The two hormones dilate blood vessels, increase the heart and respiratory rate, and suppress the digestive and immune systems. These responses boost the body’s transport of oxygen to the brain and muscles, thereby improving the body’s ability to fight or flee (Open Stax, 2022).
The Hypothalamus–Pituitary Complex
The hypothalamus–pituitary complex can be thought of as the “command center” of the endocrine system. This complex secretes several hormones that directly produce responses in target tissues, as well as hormones that regulate the synthesis and secretion of hormones of other glands. In addition, the hypothalamus–pituitary complex coordinates the messages of the endocrine and nervous systems. In many cases, a stimulus received by the nervous system must pass through the hypothalamus–pituitary complex to be translated into hormones that can initiate a response. See Figure 10.1d for an illustration of the hypothalamus–pituitary complex (Open Stax, 2022).
The hypothalamus connects to the pituitary gland by the stalk-like infundibulum. The pituitary gland consists of an anterior and posterior lobe, with each lobe secreting different hormones in response to signals from the hypothalamus.
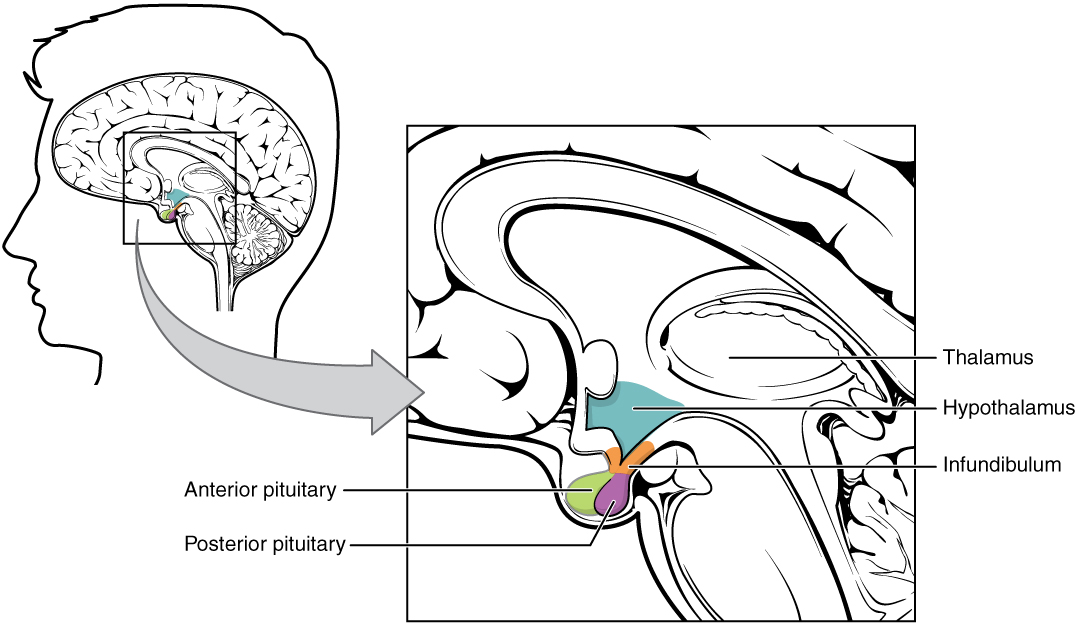
The Pituitary Gland and its Hormones
The pituitary is a gland about the size of a small marble and is located in the brain directly below the hypothalamus. The pituitary gland consists of two parts: the anterior pituitary and the posterior pituitary.
Posterior Pituitary
The posterior pituitary gland does not produce hormones, but stores and secretes two hormones produced by the hypothalamus: oxytocin and antidiuretic hormone (ADH).
Oxytocin
Oxytocin stimulates contractions in the uterus during childbirth. In nursing women, the hormone activates milk ejection or the let-down reflex.
Antidiuretic Hormone (ADH)
The antidiuretic hormone, is regulated by the osmolality of the plasma and it is also regulated by baroreceptors in response to hypovolemia and low arterial blood pressure. ADH is released in response to increased serum osmolality and decreased blood pressure, resulting in the reabsorption of water from the urine in the kidney (Copstead & Banasik, 2010).
Blood osmolarity, the concentration of sodium ions and other solutes, is constantly monitored by osmoreceptors in the hypothalamus. Blood osmolarity may change in response to the consumption of certain foods and fluids, as well as in response to disease, injury, medications, or other factors. In response to high blood osmolarity, which can occur during dehydration or following a very salty meal, the osmoreceptors signal the posterior pituitary to release antidiuretic hormone (ADH). Its effect is to cause increased water reabsorption by the kidneys. As more water is reabsorbed by the kidneys, a greater amount of water is returned to the blood, thus causing a decrease in blood osmolarity. The release of ADH is controlled by a negative feedback loop. As blood osmolarity decreases, the hypothalamic osmoreceptors sense the change and prompt a corresponding decrease in the secretion of ADH. As a result, less water is reabsorbed by the kidneys.
Drugs can also affect the secretion of ADH or imitate its effects. For example, alcohol consumption inhibits the release of ADH, resulting in increased urine production that can eventually lead to dehydration and a hangover. Vasopressin is a synthetic ADH medication used to treat very low blood pressure. It is called vasopressin because in very high concentrations it also causes constriction of blood vessels in addition to the retention of water. Vasopressin is also used to treat a disease called diabetes insipidus (DI) that causes dehydration due to an underproduction of ADH (Open Stax, 2022).
Anterior Pituitary
In contrast to the posterior pituitary, the anterior pituitary does manufacture hormones. There are seven hormones it produces and can be divided into two categories. These hormones either:
- Directly affect target organs. These two hormones are growth hormone (GH) and prolactin.
- GH stimulates somatic growth and regulates metabolism.
- Prolactin stimulates breast tissue development and lactation and suppresses reproductive function. Prolactin is also released during sexual activity and stress.
- Stimulate target glands (i.e. adrenal glands, gonads, thyroid gland) to produce target gland hormones.
- thyroid-stimulating hormone (TSH),
- adrenocorticotropic hormone (ACTH),
- follicle-stimulating hormone (FSH),
- luteinizing hormone (LH),
- beta endorphin
Of the hormones of the anterior pituitary, TSH, ACTH, FSH, and LH are collectively referred to as tropic hormones (trope- = “turning”) because they turn on or off the function of other endocrine glands.
The secretion of hormones from the anterior pituitary is regulated by two classes of hormones secreted by the hypothalamus. These are called releasing hormones and inhibiting hormones. They both help regulate growth, metabolism and reproduction. For example, thyrotropes release TSH in response to hypothalamic thyrotropin releasing hormone (TRH). An example of an inhibiting hormone is dopamine, that inhibits the release of prolactin, reducing lactation until needed (Copstead & Banasik, 2010). See Figure 10.1e to review the role of releasing hormones.
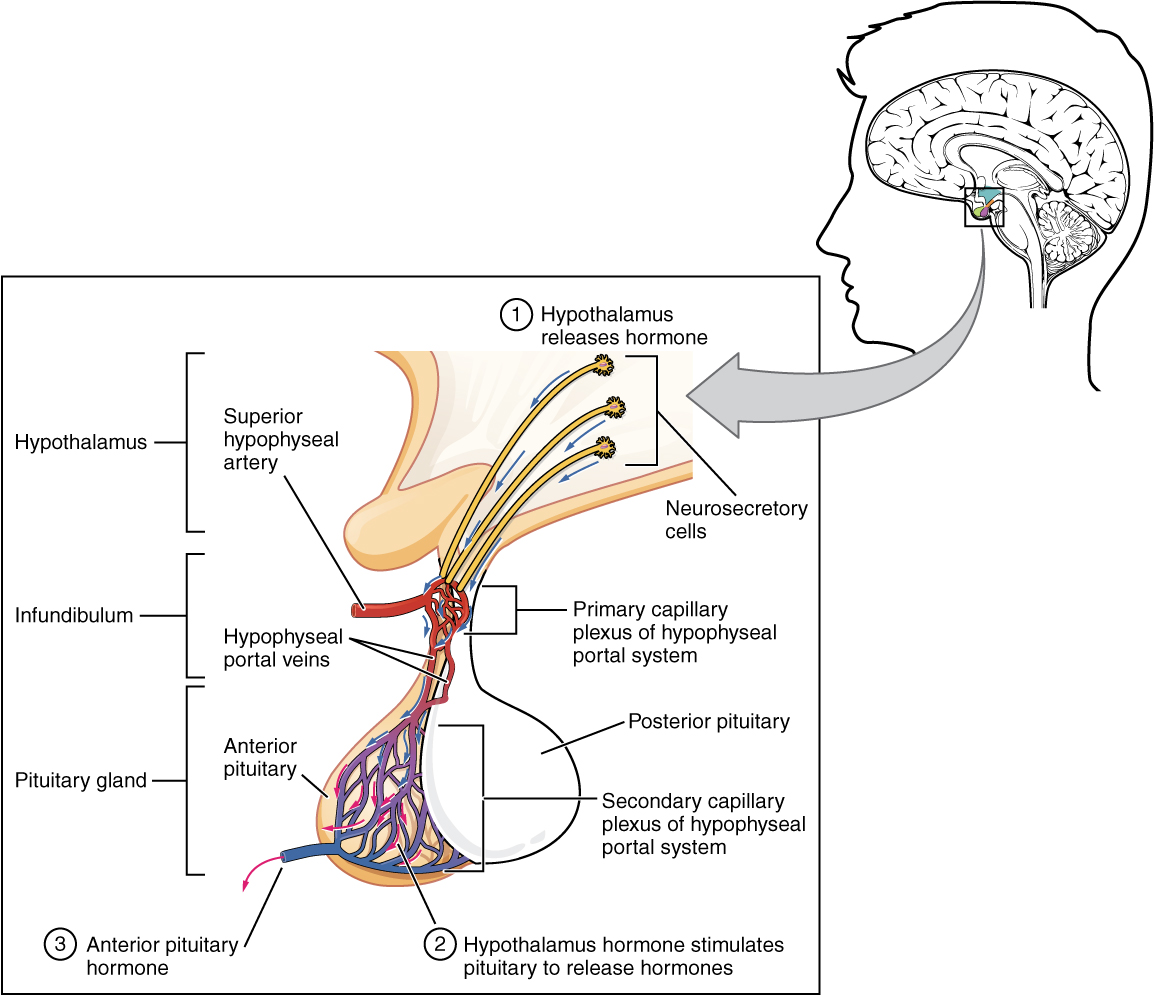
Of the anterior pituitary hormones, this unit will focus on the effects of TSH and ACTH.
Thyroid-Stimulating Hormone (TSH)
The activity of the thyroid gland is regulated by the thyroid-stimulating hormone (TSH). TSH is released from the anterior pituitary in response to the thyrotropin-releasing hormone (TRH) from the hypothalamus and triggers the secretion of thyroid hormones by the thyroid gland. In a classic negative feedback loop, elevated levels of thyroid hormones in the bloodstream then trigger a drop in production of TRH and subsequently, the production of TSH. TSH is further discussed in the “Thyroid” submodule.
Adrenocorticotropic Hormone (ACTH)
The adrenocorticotropic hormone (ACTH) is released from the anterior pituitary in response to the corticotropin-releasing hormone (CRH) from the hypothalamus. ACTH then stimulates the adrenal cortex to secrete corticosteroid hormones such as cortisol. A variety of stressors can also influence the release of ACTH, and the role of ACTH in the stress response is discussed under the “Adrenal” submodule (Open Stax, 2022).
Watch the supplementary video about ACTH and the adrenal gland is provided below. ACTH and the Adrenal Gland
Forciea, B. (2015, May 12). Anatomy and Physiology: Endocrine System: ACTH (Adrenocorticotropin Hormone) V2.0. [Video]. YouTube. All rights reserved. Video used with permission. https://youtu.be/4m7XflJzm2w. ↵
Adrenal Glands
The adrenal glands are located on top of the kidneys, and consists of the adrenal cortex that is composed of glandular tissue and the adrenal medulla that is composed of nervous tissue. Each region secretes its own set of hormones.
- Adrenal cortex: hormones released are glucocorticoids, mineralocorticoids and androgens.
- Adrenal medulla: hormones released are epinephrine and norepinephrine.
One of the major functions of the adrenal gland is to respond to stress. The body responds in different ways to short-term stress and long-term stress, following a pattern known as the general adaptation syndrome (GAS). Stage one of GAS is called the alarm reaction. This is short-term stress, also called the fight-or-flight response, and is mediated by the hormones epinephrine and norepinephrine from the adrenal medulla. Their function is to prepare the body for extreme physical exertion. If the stress is not soon relieved, the body adapts to the stress in the second stage called the stage of resistance. If a person is starving for example, the body may send signals to the gastrointestinal tract to maximize the absorption of nutrients from food. If the stress continues for a longer term however, the body responds with symptoms such as depression, suppressed immune response, or severe fatigue. These symptoms are mediated by the hormones of the adrenal cortex, especially cortisol. Adrenal hormones also have several non–stress-related functions, including the increase of blood sodium and glucose levels, which will be described in further detail below.
Adrenal Cortex
The adrenal cortex is a component of the hypothalamic-pituitary-adrenal (HPA) axis. The hypothalamus stimulates the release of ACTH from the pituitary, which then stimulates the adrenal cortex to produce steroid hormones and include glucocorticoids (cortisol), mineralocorticoids (aldosterone), and the sex hormones (androgens). Steroid hormones travel in the circulation bound to proteins and diffuse through their target cell membranes and then binding with their cytoplasmic receptors. These hormones, and especially cortisol, are essential for life. They are important for the regulation of the stress response, blood pressure and blood volume, nutrient uptake and storage, fluid and electrolyte balance, and inflammation (Copstead & Banasik, 2010).
We will review each of the three types of hormones.
Mineralocorticoids: Aldosterone
The most superficial region of the adrenal cortex is the zona glomerulosa, which produces a group of hormones collectively referred to as mineralocorticoids because of their effect on body minerals, especially sodium and potassium. These hormones are essential for fluid and electrolyte balance.
Aldosterone is the major mineralocorticoid that is important in the regulation of the concentration of sodium and potassium ions in the body. Or, in other words, to maintain normal salt and water balance in the body. To do this, aldosterone promotes sodium retention and potassium excretion at the distal renal tubules (Copstead & Banasik, 2010).
The secretion of aldosterone by the adrenal cortex is prompted by the HPA axis when the hypothalamus triggers ACTH release from the anterior pituitary. It is released in response to elevated blood levels of potassium (K+), low blood levels of sodium (Na+), low blood pressure, or low blood volume. Aldosterone targets the kidneys and increases the excretion of K+ and the retention of Na+, which, in turn, causes the retention of water, thus increasing blood volume and blood pressure.
Aldosterone is also a key component of the renin-angiotensin-aldosterone system (RAAS) in which specialized cells of the kidneys secrete renin in response to low blood volume or low blood pressure. Renin then catalyzes the conversion of the blood protein angiotensinogen, which is produced by the liver, to the hormone Angiotensin I. Angiotensin I is converted in the lungs to Angiotensin II by the angiotensin-converting enzyme (ACE).
Angiotensin II has three major functions:
- initiating vasoconstriction of the arterioles, thus decreasing blood flow;
- stimulating kidney tubules to reabsorb sodium and water, thus increasing blood volume;
- signaling the adrenal cortex to secrete aldosterone, which further increases blood volume and blood pressure.
It is important to understand these effects because many cardiac medications target the effects of aldosterone and the RAAS system. For example, drugs that block the production of Angiotensin II are known as ACE inhibitors. ACE inhibitors are used to help lower blood pressure in clients with hypertension by blocking the ACE enzyme from converting Angiotensin I to Angiotensin II, which, in turn, causes vasodilation of the arterioles. Another medication called spironolactone is used as a diuretic because it blocks the effects of aldosterone and, thus, causes the kidneys to eliminate water and sodium to decrease blood volume and blood pressure. Refer to the diagram of the Renin-Angiotensin-Aldosterone System, figure 10.1e.
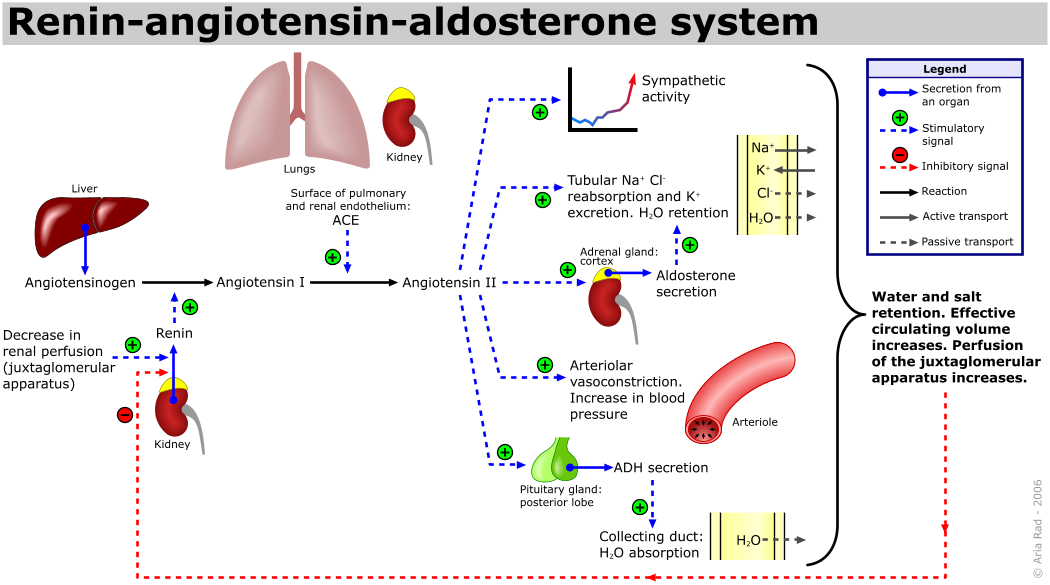
File:Renin-angiotensin-aldosterone system.png File:Renin-angiotensin-aldosterone system.png – Wikimedia Commons
Glucocorticoids: Cortisol
The intermediate region of the adrenal cortex produces hormones called glucocorticoids because of their role in glucose metabolism. Glucocorticoids, primarily cortisol, affects nearly every tissue in the body and has a broad range of effects. In simple terms, it has a role in the metabolism of fats, proteins and carbohydrates, it suppresses inflammation, regulates blood pressure, increases blood sugar, alters mood and behaviour, and helps control your sleep-wake cycle. If a person is stressed, cortisol is released to give your body the energy boost. Some of the physiological effects of cortisol include:
- increases glucose levels in the blood by stimulating gluconeogenesis in the liver and promotes the formation of glycogen in the liver.
- contributes to protein catabolism by releasing muscle stores of proteins, providing amino acids for glucose production in the liver.
- promotes lipolysis and increased blood cholesterol levels
- reduces glucose uptake into muscle and adipose tissue, thereby opposing the effects of insulin and raising blood sugar.
- promotes protein and lipid breakdown into products, amino acids and glycerol, respectively, that can be used for gluconeogenesis in the liver.
- regulates inflammatory and immune responses to protect against the damaging effects of stress. (Copstead & Banasik, 2010, Open Stax, 2022).
In response to long-term stressors, the HPA axis triggers the release of glucocorticoids. Their overall effect is to inhibit tissue building while stimulating the breakdown of stored nutrients to maintain adequate fuel supplies. In conditions of long-term stress, cortisol promotes the catabolism of glycogen to glucose, stored triglycerides into fatty acids and glycerol, and muscle proteins into amino acids. These raw materials can then be used to synthesize additional glucose and ketones for use as body fuels. However, the negative effects of catabolism for energy can result in muscle breakdown and weakness, poor wound healing, and the suppression of the immune system.
It is likely clear that cortisol is a vital hormone in the response to acute stress, such as from infection, injury, hypoglycemia or emotional stress. These stressors lead to an increase in cortisol levels in the blood. Glucocorticoids are often given to treat conditions such as acute inflammation, overactive immune system or high levels of cortisol. For example, glucocorticoids will suppress tissue inflammation such as a cortisone injection into an inflamed joint or giving steroid-based inhalers to manage inflammation that occurs in asthma.
Androgens
The deepest region of the adrenal cortex produces small amounts of a class of steroid sex hormones called androgens. During puberty and most of adulthood, androgens are produced in the gonads. The androgens produced in the adrenal cortex supplement the gonadal androgens.
Adrenal Medulla
The adrenal medulla is neuroendocrine tissue composed of postganglionic sympathetic nervous system (SNS) neurons, that secretes the hormones epinephrine and norepinephrine. It is an extension of the autonomic nervous system, which regulates homeostasis in the body. See Figure 10.1g for an illustration of the adrenal gland and associated hormones.
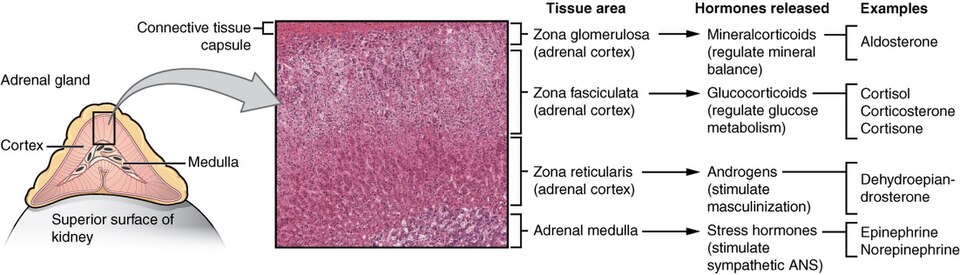
Epinephrine and Norepinephrine
As noted earlier, the adrenal cortex releases glucocorticoids in response to long-term stress such as severe illness. In contrast, the adrenal medulla releases its hormones in response to acute, short-term stress mediated by the sympathetic nervous system (SNS). The medullary tissue is composed of unique postganglionic SNS neurons called chromaffin cells that produce the neurotransmitters epinephrine (also called adrenaline) and norepinephrine (also called noradrenaline), which are chemically classified as catecholamines. Epinephrine is produced in greater quantities and is the more powerful hormone.
The secretion of medullary epinephrine and norepinephrine is controlled by a neural pathway that originates from the hypothalamus in response to danger or stress. Both epinephrine and norepinephrine increase the heart rate, pulse, and blood pressure to prepare the body to fight the perceived threat or flee from it. In addition, the pathway dilates the airways, raising blood oxygen levels. It also prompts vasodilation, further increasing the oxygenation of important organs such as the lungs, brain, heart, and skeletal muscle while also prompting vasoconstriction to blood vessels serving less essential organs such as the gastrointestinal tract, kidneys, and skin. It also downregulates some components of the immune system. Other effects include a dry mouth, loss of appetite, pupil dilation, and a loss of peripheral vision.
In summary, there are many hormones that regulate the metabolic functions of our bodies. These hormones are influenced by a number of factors including circadian rhythms, hormone release from target cells, stress and pain. Endocrine disorders can be related to hyposecretion, hypersecretion and target cell hyperresponsiveness. We will explore some of these disorders in the next unit.
Interactive Activity
Media Attributions
- 10.1a “1801 The Endocrine System.jpg“
- 10.1b “1805 Negative Feedback Loop.jpg“
- 10.1c “1806 The Hypothalamus-Pituitary Complex.jpg“
- 10.1d “1808 The Anterior Pituitary Complex.jpg“
- 10.1e The hypothalamus releases hormones to regulate the release of hormones from the anterior pituitary. File:1808 The Anterior Pituitary Complex.jpg File:1808 The Anterior Pituitary Complex.jpg – Wikimedia Commons
- 10.1f The renin–angiotensin system (RAS), or renin–angiotensin–aldosterone system (RAAS), is a hormone system that regulates blood pressure, fluid, electrolyte balance, and systemic vascular resistance. Retrieved from File:Renin-angiotensin-aldosterone system.png File:Renin-angiotensin-aldosterone system.png – Wikimedia Commons
- 10.1g The Adrenal Gland and Associated Hormones File:1818 The Adrenal Glands.jpg File:1818 The Adrenal Glands.jpg – Wikimedia Commons
References
- Copstead, L. & Banasik, J. (2010). Pathophysiology (4th ed.). Missouri: Elsevier.
- Forciea, B. (2015, May 12). Anatomy and Physiology: Endocrine System: ACTH (Adrenocorticotropin Hormone) V2.0. [Video]. YouTube. All rights reserved. Video used with permission. https://youtu.be/4m7XflJzm2w
- Giddens, J. (2017). Concepts of Nursing Practice (2nd ed.). Missouri: Elsevier.
- Hiller-Stumhofel, S. & Bartke, A. (1998). The Endocrine System. An overview. Alcohol Health and Research World, 22(3), 153-164.PMCID: PMC6761896 PMID: 15706790
- Open Stax (2022). Anatomy and Physiology. OpenStax licensed under CC BY 4.0. Access for free at https://openstax.org/books/anatomy-and-physiology/pages/1-introduction ↵

