1.5 Pharmacokinetics — Metabolism (Biotransformation) V2
Once a drug has been absorbed and distributed in the body, it will then be broken down by a process known as metabolism. Metabolism is the process of chemically converting a drug into a form that can be more easily removed from the body (Adams et al., 2019, p. 23). Most drug metabolism takes place in the liver. Other organs that aid in metabolism include the kidneys, skeletal muscles, lungs, plasma, and intestinal mucosa. Very few drugs are not metabolized in the liver such as gabapentin or digoxin.
Everything that enters the bloodstream—whether swallowed, injected, inhaled, absorbed through the skin, or produced by the body—is carried to the liver. Very simply, most drugs or substances (vitamins, minerals, nutrients) will be transformed by hepatic enzymes into polar metabolites, inactivating the drug and allowing it to be more easily excreted in the urine or bile.
More specifically, there are two phases to metabolism:
- The hepatic microsomal enzyme system uses oxidation, reduction, and hydrolysis reactions to make the drug slightly more polar (water soluble).
- Conjugation with endogenous substrates further changes the drug into a polar metabolite that is then inactive and easily excreted.
Hepatic Microsomal Enzyme System
The hepatic microsomal enzyme system, also known as the P450 system, is capable of catalyzing a variety of chemical reactions and aiding in the metabolism of medications. The primary effect of the enzymes is in accelerating renal excretion of a drug. These enzymes target lipid-soluble, non-polar drugs as they are difficult to eliminate and include the majority of the drugs. Converting lipid-soluble drugs into polar metabolites renders them less able to enter the tissues. Water-soluble medications are easily metabolized by simpler metabolic reactions such as hydrolysis.
P450 enzymes catalyze many reactions resulting in several different outcomes, including:
- accelerated renal excretion of drugs,
- drug inactivation,
- increased therapeutic action by prodrug activation (e.g., codeine is converted into morphine to enable pain relief, and losartan, an antihypertensive med, has no therapeutic activity until metabolized into an active form), and
- increased or decreased toxicity (e.g., acetaminophen is converted into a hepatotoxic form that is safe in therapeutic doses, but toxic in an overdose). (Adams et al., 2019; Le, 2024)
P450 System

The chromosome P450 is a group of 12 closely related enzyme families. Three of the P450 (CYP) families—CYP1, CYP2, CYP3—metabolize drugs. The other nine families metabolize other compounds such as steroids or fatty acids. Each of the three CYP families are also composed of multiple forms and metabolize certain drugs. They are identified by additional letters and numbers, for example, CYP2D6 and CYP3A4.
Each metabolize different drugs; for example, CYP3A4 metabolizes many drugs including acetaminophen, codeine, and erythromycin. It is actually the most abundant cytochrome in the liver and intestinal tract, and accounts for 30–40% of cytochrome activity.
Inducers and Inhibitors
Further, CYP450 enzymes can be induced or inhibited by many drugs and substances, resulting in drug interactions in which one drug enhances the toxicity or reduces the therapeutic effect of another drug.
Example: The drug Verapamil (a calcium-channel blocker) will inhibit the CYP3A4 enzyme, leading to increased drug effects and risk of side effects for some drugs.
Example: Phenobarbital is a CYP3A4 inducer, so it increases the rate of its own metabolism and of other drugs. Therefore, higher doses may be required to achieve a therapeutic effect.
Inducers and inhibitors are not just prescription or OTC drugs but can also be other substances, such as herbal remedies. St. John’s Wort, an easily available herbal remedy, sometimes used for depression. It is a powerful CYP3A4 inducer, resulting in many medication to break down quickly and becoming less effective. It should not be taken with antidepressants, birth control, anticoagulants or immunosuppressants (National Center for Complimentary and Integrative Health, 2025). Nurses must always ask about clients about any supplements or herbal remedies they may be taking to avoid unwanted lower therapeutic effects.
First-Pass Effect
One of the first steps in metabolizing drugs occurs through a process known as the first-pass effect, in which orally administered drugs are broken down in the liver and intestines. This makes the substance easier to excrete in the urine. Medications made of protein that are swallowed or otherwise absorbed in the GI tract may quickly be deactivated by enzymes as they pass through the stomach and duodenum. If the drug enters the blood from the intestines, part of it will be broken down by liver enzymes, known as the first-pass effect, and some of it will escape to the general circulation to either be protein-bound (inactive) or stay free (and create an action at a receptor site). Thus, several doses of an oral medication may be needed to maintain enough active free drug in the circulation to exert the desired effect. Refer to 1.2 Absorption for further information about first-pass effect.
Some drugs undergo rapid hepatic metabolism via first-pass effect that leaves the drug ineffective or with a low bioavailability. In these cases, the drug will be administered intravenously so it avoids first-pass effect. For example, Morphine given orally undergoes extensive first pass metabolism. If given as the same dose as IV, there will be very low bioavailability with low therapeutic response. Therefore, the dose is adjusted to a 3:1 ratio. Morphine 30 mg po = Morphine 10 mg IV.
The Effect of Food on Metabolism
The metabolism of a drug can be impacted by other drugs, food, or supplements. Often, these drug-substance interactions are unintentional from accidental misuse or lack of knowledge. While drug-drug interactions are more widely researched, food-drug interactions are less known.
Some more common interactions include:
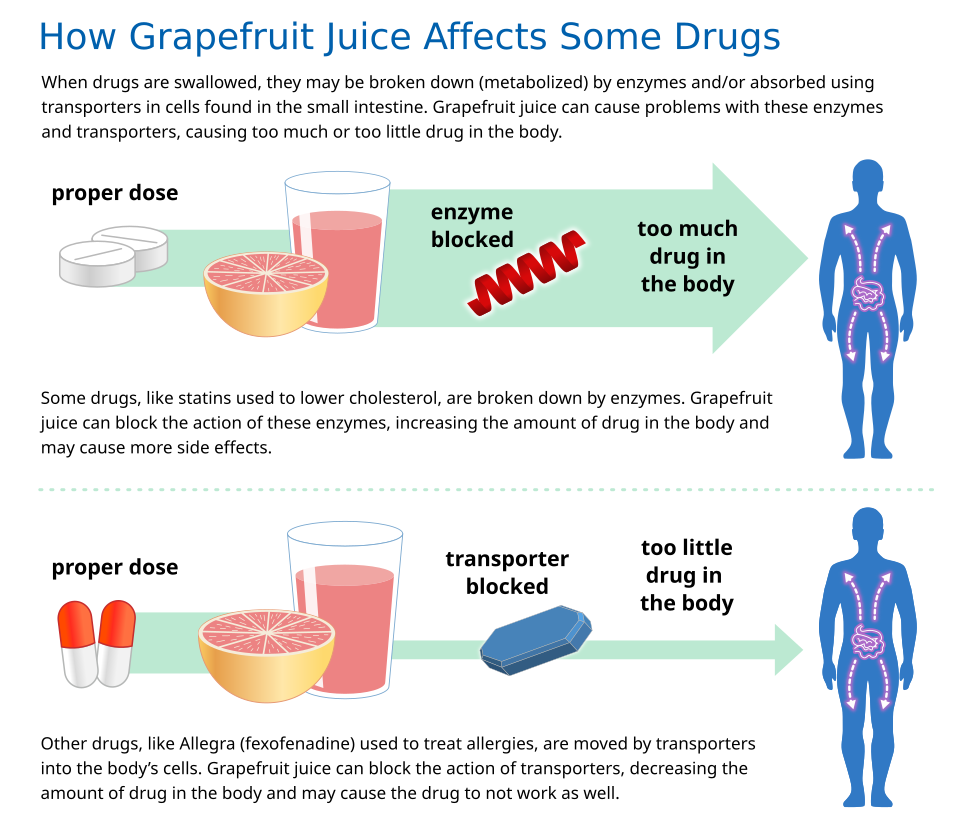
- Grapefruit Juice: Grapefruit juice (GFJ) is unique among juices as it inhibits CYP3A enzymes due to the Furanocoumarins in the juice. This can lead to an increase in oral bioavailability of medications that are CYP 3A4 substrates—like felodipine for high blood pressure or midazolam, a sedative—which can raise their concentrations above toxic levels (Bushra et al., 2011). (See below: Do you know the power of Grapefruit Juice?.)

- Dietary Protein: Warfarin, an anticoagulant, can be impacted by dietary protein, which can raise serum albumin levels and P450 activity, leading to a decrease in the international normalized ratio (INRs). Vitamin K rich foods can also impact warfarin levels, so clients are advised to take consistent levels of vitamin K foods (leafy greens, avacados, soy).
Thus, dietary considerations must be considered for clients taking medications that have a narrow therapeutic window or are higher-risk medications. They need to be fully informed of any potential interactions so they can take an active role in avoiding drug-food interactions.
Lifespan Considerations
Neonate and Pediatric: The developing liver in infants and young children produces decreased levels of microsomal enzymes. Because of this, a young child or neonate may have a decreased ability to metabolize medications. In contrast, older children may experience increased metabolism and require higher doses of medications once the hepatic enzymes are fully produced (Fernandez et al., 2011). Always exercise caution when administering medications to children and infants.
Older Adult: Hepatic metabolism may decline in older adults. As a result, dosages should be adjusted according to the client’s liver function and anticipated metabolic rate. First-pass metabolism also decreases with aging; therefore, older adults may have higher “free” circulating drug concentrations and be at a higher risk for side effects and toxicities (Fernandez et al., 2011).
Putting It All Together
Drugs can be metabolized by a number of processes, including oxidation, hydrolysis, conjugation, condensation, or isomerization, resulting in drug molecules transforming into smaller molecules, transforming into polar metabolites, or in some cases, synthesizing into a larger prodrug. Once liver enzymes have completed metabolizing a drug, the now-inactive drug undergoes the final stage of its time in the body—excretion—as it exits via the urine or feces.
Clinical Reasoning and Decision Making Activities
Metabolism can be influenced by many factors within the body. If a client has liver damage, the client may not be able to break down (metabolize) medications as efficiently. Dosages are calculated according to the liver’s ability to metabolize and the kidney’s ability to excrete.
- When caring for a client with cirrhosis, how does this condition impact the dosages prescribed for the client? What should be nurse be monitoring or evaluating?
Note: Answers to the Clinical Reasoning activities can be found in the “Answer Key” sections at the end of the book.
Did You Know the Power of Grapefruit Juice?
A Juicy Story
Did you know that, in some people, a single glass of grapefruit juice can alter levels of drugs used to treat allergies, heart diseases, and infections? Fifteen years ago, pharmacologists discovered this “grapefruit juice effect” by luck, after giving volunteers grapefruit juice to mask the taste of a medicine. Nearly a decade later, researchers figured out that grapefruit juice affects the metabolizing rates of some medicines by lowering levels of a drug-metabolizing enzyme, called CYP3A4 (part of the CYP450 family of drug-binding enzymes), in the intestines.
More recently, Paul B. Watkins of the University of North Carolina at Chapel Hill discovered that other juices like Seville (sour) orange juice—but not regular orange juice—have the same effect on the liver’s ability to metabolize using enzymes. Each of ten people who volunteered for Watkins’ juice-medicine study took a standard dose of felodopine (Plendil), a drug used to treat high blood pressure, diluted in grapefruit juice, sour orange juice, or plain orange juice. The researchers measured blood levels of Plendil at various times afterward. The team observed that both grapefruit juice and sour orange juice increased blood levels of Plendil, as if the people had received a higher dose. Regular orange juice had no effect. Watkins and his coworkers have found that a chemical common to grapefruit and sour oranges, dihydroxybergamottin, is likely the molecular culprit.
Thus, when taking medications that use the CYP3A4 enzyme to metabolize, clients are advised to avoid grapefruit juice and sour orange juice.
Davis, 2006
References
Adams, M., Urban, C., El-Hussein, M., Osuji, J., & King, S. (2018). Pharmacology for nurses. A pathophysiological approach (2nd Canadian ed.). Pearson.
Burcham, J. R., & Rosenthal, L. (2019). Lehne’s pharmacology for nursing care (10th ed.). Elsevier.
Bushra, R., Aslam, N., & Khan, A. (2011). Food-drug interactions. Oman Medical Journal, 26(2), 77–83. https://doi.org/10.5001/omj.2011.21
Davis, A. (2006). Medicines by design [PDF]. National Institute of General Medical Services. https://files.eric.ed.gov/fulltext/ED507558.pdf
Fernandez, E., Perez, R., Hernandez, A., Tejada, P., Arteta, M., & Ramos, J. T. (2011). Factors and mechanisms for pharmacokinetic differences between pediatric population and adults. Pharmaceutics, 3(1), 53–72. https://doi.org/10.3390/pharmaceutics3010053
Le, J. (2024). Drug excretion. Merck Manual. https://www.merckmanuals.com/professional/clinical-pharmacology/pharmacokinetics/drug-excretion
National Center for Complimentary and Integrative Health (2025). St. John’s Wort. St. John’s Wort: Usefulness and Safety | NCCIH
Media Attributions
Figure 1.5a Cytochrome Nomenclature.png (https://commons.wikimedia.org/wiki/File:Cytochrome_Nomenclature.png) by Mohmmed Laique, Wikimedia Commons CC BY-SA 4.0
Figure 1.5b “Grapefruit” by Marco Verch, Pixabay, Pixabay Content License
Figure 1.5c Grapefruit Juice and Medicine May Not Mix. File:Grapefruit Juice and Medicine May Not Mix (6774935740) – en.svg – Wikimedia Commons by FDA graphic by Michael J. Ermarth, Wikimedia Commons, CC BY-SA 4.0
The breakdown of a drug molecule via enzymes in the liver (primarily) or intestines (secondarily).
The breakdown of orally administered drugs in the liver and intestines.

