6.3 Clinical Reasoning and Decision-Making for Pain and Mobility
Clinical reasoning is a way that nurses think and process our knowledge, including what we have read or learned in the past, and apply it to the current practice context of what we are seeing right now (NCSBN, n.d). Nurses make decisions all the time but making decisions requires a complex thinking process. There are many tools that are useful and found online that can support your thinking through to clinical judgments. This book uses the nursing process and clinical judgment language to help you understand the application of medication to your clinical practice.
After reviewing basic concepts related to pain and several disorders requiring analgesic or musculoskeletal medication, it is time to consider how to make decisions about these types of medications.
Assessment
Although there are numerous details to consider when administering medications, it is always important to first think about what you are giving and why.
First, let’s think of why? Recognizing Cues
Prior to administration of any medication, nurses should perform an assessment and gather cues to analyze and prioritize a hypothesis (Tanner, 2006).
For instance, if considering a pain medication, you will want to complete a full pain assessment such as determining a pain scale and acceptable pain level for your client. See Figure 6.3a[1] for common nursing mnemonics for pain assessment.
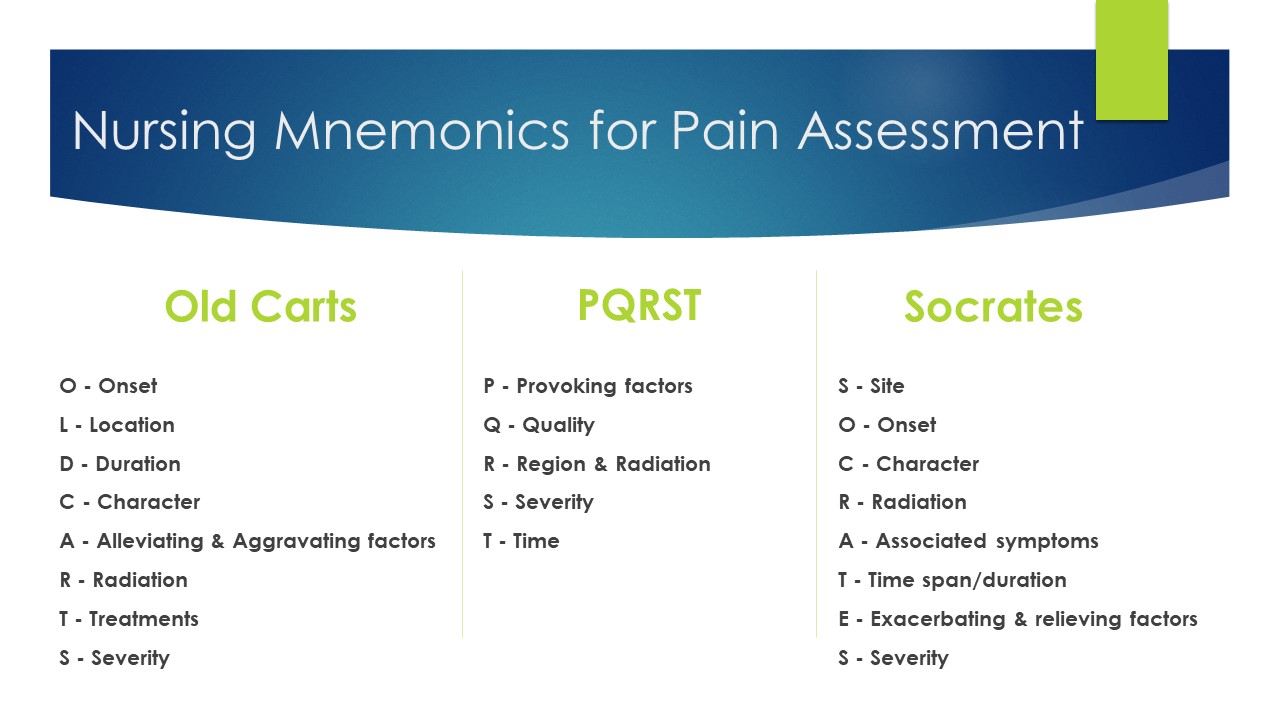
If administering a medication related to mobility or the musculoskeletal system, you will first want to collect data such as strength and stability.
Additional baseline information to collect prior to administration of any analgesic or musculoskeletal medication includes health history, history of similar pain and treatments, history of allergies to medications or a previous adverse response.
Other cues:
Clients with pain will often have other cues that alert us to the intensity of pain. For acute pain, it can be mild to severe. Some cues during acute pain can include:
- Vital signs: tachycardia, tachypnea, elevated blood pressure, and shallow breathing. If the rate of breathing is elevated and compromised, this may lead to lower oxygen saturations. Diaphoresis and elevated temperature may also be seen.
- Gastrointestinal: nausea, vomiting and constipation may occur. This is due to changes to digestion and GI upset.
- other: increased blood glucose levels due to the stress response
For chronic pain, that is long term in nature, some of the physical symptoms are no longer present. But clients may experience disrupted sleep, fatigue, and depression.
Understanding types of pain
To be able to adequately assess and treat a client’s pain, nurses need to understand the type of pain a client may be experiencing. Different types of pain will present differently and will be treated differently. For example, neuropathic pain versus acute post op pain. The types of pain include neuropathic, acute, and chronic. A client with neuropathic pain which is caused by nerve damage may feel a burning or tingling sensation. Post-operative pain will be a sharp pain but with a short duration.
Lifespan Considerations
A majority of medications are calculated specifically based on the client’s size, weight, and renal function. Client age and size are especially vital in pediatric clients. A child’s stage of development and the size of their internal organs will greatly impact how the body absorbs, digests, metabolizes and eliminates medications.
Visual pain scales have been developed as a tool of communication about pain with children and adults. The Wong-Baker pain scale was the first developed to provide a visual representation of a client’s pain level. The one that is presented below, figure 6.3b for the FACES Pain Rating Scale, can be used for clients over the age of 3. To use this scale, use the following evidence-based instructions.
- Explain to the client that each face represents a person who has no pain (hurt), some, or a lot of pain.
- Explain, “Face 0 doesn’t hurt at all. Face 2 hurts just a little. Face 4 hurts a little more. Face 6 hurts even more. Face 8 hurts a whole lot. Face 10 hurts as much as you can imagine, although you don’t have to be crying to have this worst pain.”
- Ask the client to choose the face that best represents the pain they are feeling.
![Wong-Baker FACES Foundation (2020). Wong-Baker FACES® Pain Rating Scale. Retrieved [Date] with permission from http://www.WongBakerFACES.org Image of Wong-Baker FACES pain rating scale](http://fundamentals-nursing-pharmacology-2e-ca.pressbooks.tru.ca/wp-content/uploads/sites/251/2025/02/image6-4.png)
Determinants of Health and Cultural Safety
There are several considerations for nurses when working with clients who have conditions related to pain and mobility. It is important that you engage in client care that is culturally safe, remember that pain is what the client says it is, and not further marginalize clients (Craig et al, 2020).
Interventions
Next, plan (refine your hypothesis), and take action.
Once you have gathered your assessment data and cues, you’ll begin to generate solutions to the concern that your client has. Prior to administration, it is important to consider the best route of administration for this client at this particular time. For example, if the client is nauseated and vomiting, then an oral route may not be effective.
There are also legal and ethical considerations when administering some analgesics such as opioids. When administering opioid medications, it is important to remember that these medications are controlled substances with special regulations regarding storage, auditing counts, and disposal or wasting of medication. Read more information about controlled substances in Chapter 2.
In general, when administering analgesics, we often will use the least invasive medication that is anticipated to treat the level of pain reported by the client. The World Health Organization (WHO) pain ladder was originally developed for the selection of analgesics for clients with cancer but illustrates the step-wise approach to pain control based on the level of pain indicated by the client. See Figure 6.3c for an image of the WHO ladder. For example, if a client reports a pain level of “2,” then it is appropriate to start at the lowest rung of the ladder and administer a non-opioid. However, it may be clinically indicated to start at “Level 3” on the WHO ladder for clients who present with severe, difficult pain. This model is very simplistic and does not take into account clinical context or client factors. But, it is still relevant today with the step up-step down approach to pain management.

It is important to anticipate any common side effects and the expected outcome of the medication, as well as considerations regarding what to teach the client and their family regarding the medications. This information will be dependent upon the medication.
Evaluation
Finally, evaluate the outcomes of your action.
It is important to always evaluate the client’s response to a medication. In most circumstances, the nurse should assess for a decrease in pain 30 minutes after intravenous (IV) administration and 60 minutes after oral medication. If the client’s pain level is not acceptable, the nurse should investigate alternate treatment modalities or repeated or increased dosage depending on client factors and type of analgesia. Alternative treatment modalities may include, but are not limited to aromatherapy, repositioning the client, hot or cold treatments, and listening to music.
As the nurse is the client’s advocate, the healthcare provider may have to be informed if the client’s pain is not being controlled by analgesics. Nurses should also evaluate for any adverse effects. For instance, one adverse effect of opioid analgesics is respiratory depression. The nurse should evaluate the respiratory rate and pulse oximetry after administration of the medication. The nurse may need to consider administering other medications that treat the side effects of analgesic medication.
Pain Management Take-Aways
- use oral analgesics whenever possible.
- give analgesics at regular intervals and breakthrough analgesia as needed.
- give analgesics based on the level of intensity of pain.
- the dosage of pain is individualized to that client
- manage and anticipate adverse effects. For example, anticipate constipation from opioids and have a plan for prevention.
Vargas-Schaffer, 2010
Interactive Activity
References
NCSBN (n.d.). NCSBN Clinical Judgement Measurement model. https://www.ncsbn.org/14798.htm[
Craig, K., Holmesm, C., Hudspith, M., Moor, G., Moosa-Mitha, M., Varcoe, C. & Wallace, B. (2020). Pain in persons who are marginalized by social conditions. Pain, 161(2). doi: 10.1097/j.pain.0000000000001719 [/footnote]
Tanner, C. (2006). Thinking like a nurse: A research-based Model of Clinical Judgement. Journal of Nursing Education 45(6). https://www.mccc.edu/nursing/documents/Thinking_Like_A_Nurse_Tanner.pdf[/
Vargas-Schaffer, G. (2010). Is the WHO analgesic ladder still valid? Canadian Family Physician,
Media Attributions
- Figure 6.3a"Mnemonics for Pain Assessment" by Julie Teeter is licensed under CC BY-SA 4.0[
- Figure 6.3b The Wong-Baker FACES Pain Rating Scale. Used with permission from http://www.WongBakerFACES.org
- Figure 6.3c. World Health Organization (1996). Cancer pain relief. 2nd ed. Geneva: WHO. for an image of the WHO ladder.
- "Mnemonics for Pain Assessment" by Julie Teeter is licensed under CC BY-SA 4.0 ↵
Cells found within the lining of the stomach that secrete mucus as a protective coating.

